Retinal Detachment: Clinical Presentation, Diagnostic Evaluation, Management, and Outcomes – A Case Report
OthersPage Navigation
Abstract
Retinal detachment is a vision-threatening ophthalmic emergency characterized by the separation of the neurosensory retina from the underlying retinal pigment epithelium. If left untreated, it can result in permanent visual impairment or blindness. Rhegmatogenous retinal detachment is the most common type and typically occurs due to retinal tears that allow vitreous fluid to accumulate beneath the retina. Early diagnosis and prompt surgical intervention are essential to preserve vision and improve anatomical outcomes.
We present the case of a 58-year-old male who presented with sudden onset flashes, floaters, and progressive painless vision loss in the left eye for 4 days. Ophthalmologic examination and fundoscopic findings confirmed rhegmatogenous retinal detachment involving the macula. The patient underwent pars plana vitrectomy with gas tamponade, resulting in successful retinal reattachment and gradual visual recovery.
This case highlights the importance of early recognition of warning symptoms, timely ophthalmologic referral, and appropriate surgical management in preventing irreversible visual loss associated with retinal detachment.
Introduction
Retinal detachment (RD) is a serious ophthalmologic condition in which the neurosensory retina separates from the retinal pigment epithelium, disrupting retinal blood supply and photoreceptor function. The condition represents an ocular emergency requiring immediate intervention to prevent permanent visual damage.
Retinal detachments are broadly classified into three major categories:
- Rhegmatogenous retinal detachment
- Tractional retinal detachment
- Exudative retinal detachment
Rhegmatogenous retinal detachment (RRD) is the most common form and occurs due to retinal breaks or tears that permit liquefied vitreous humor to enter the subretinal space. Risk factors include aging, myopia, ocular trauma, cataract surgery, and posterior vitreous detachment.
The annual incidence of retinal detachment is estimated to be approximately 10–18 cases per 100,000 individuals worldwide. The condition is more common in older adults and highly myopic individuals.
Patients commonly present with photopsia (flashes), floaters, peripheral visual field defects, or a curtain-like shadow progressing across the visual field. Macular involvement significantly affects prognosis and visual recovery.
Prompt diagnosis using dilated fundus examination and ocular imaging is crucial for successful management. Advances in vitreoretinal surgical techniques have substantially improved anatomical and functional outcomes.
Case Report
Patient History
A 58-year-old male presented to the ophthalmology emergency department with:
- Sudden onset flashes of light in the left eye
- Multiple floaters for 4 days
- Progressive painless diminution of vision
- Sensation of a dark curtain descending over the visual field
The patient denied ocular pain, redness, or discharge.
Medical history revealed:
- Hypertension for 10 years
- High myopia since childhood
- Previous cataract surgery in the left eye 3 years earlier
There was no recent history of ocular trauma.
Family history was non-contributory.
Clinical Examination
General Examination
- Patient conscious and oriented
- Blood pressure: 138/86 mmHg
- Pulse rate: 78/min
- Systemic examination unremarkable
Ophthalmic Examination
Visual Acuity
- Right eye: 6/9
- Left eye: Counting fingers at 2 meters
External Examination
- No eyelid abnormalities
- No conjunctival congestion
Pupillary Examination
- Relative afferent pupillary defect present in left eye
Slit Lamp Examination
- Clear cornea
- Deep anterior chamber
- Posterior chamber intraocular lens noted in left eye
- Mild vitreous pigment cells present
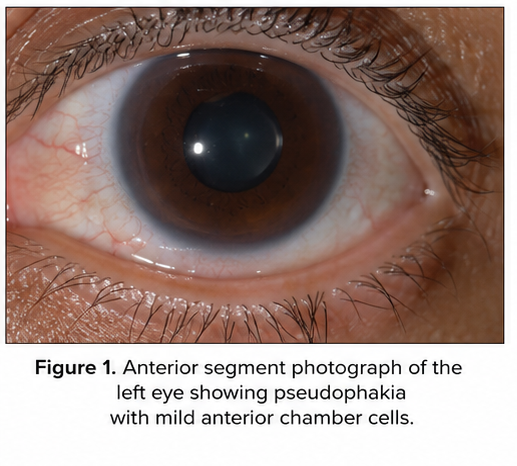
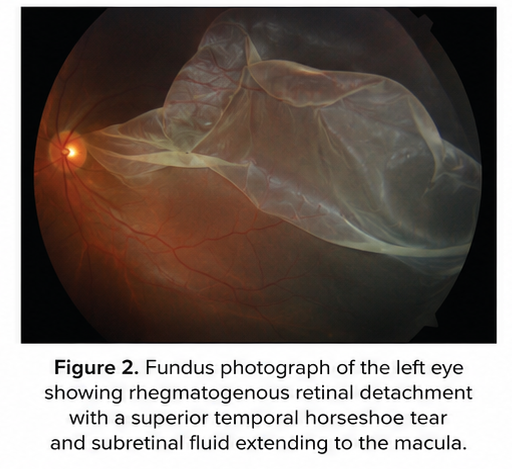
Fundus Examination
Left eye findings:
- Elevated detached retina involving superior temporal quadrant
- Horseshoe retinal tear noted
- Subretinal fluid extending toward the macula
- Macula detached
- Corrugated retinal appearance
Right eye:
- Peripheral lattice degeneration without detachment
Clinical Evaluation
Differential Diagnosis
Based on the presenting symptoms and examination findings, the following conditions were considered:
- Rhegmatogenous retinal detachment
- Posterior vitreous detachment
- Vitreous hemorrhage
- Central retinal vein occlusion
- Ocular migraine
The presence of retinal tear and detached retina confirmed retinal detachment.
Investigations
Ocular Imaging
Optical Coherence Tomography (OCT)
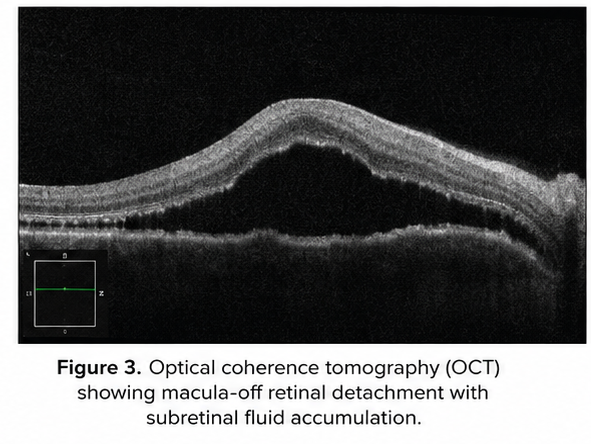
- Macular detachment confirmed
- Subretinal fluid accumulation observed
B-Scan Ultrasonography
Performed due to partial media opacity.
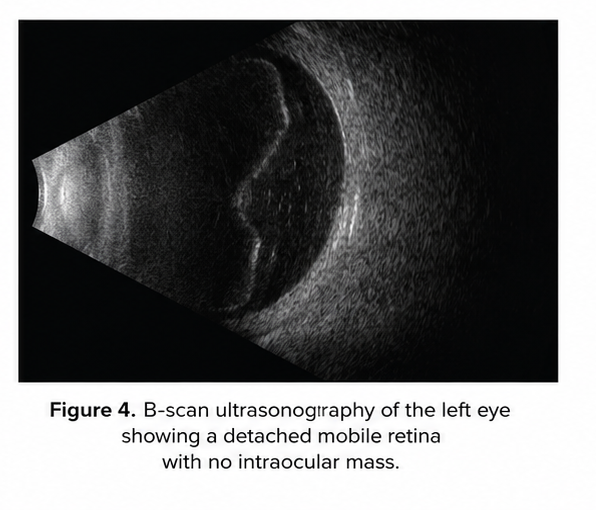
Findings included:
- Detached mobile retina
- No intraocular mass
- No vitreous hemorrhage
Routine Laboratory Tests
- Complete blood count: Normal
- Blood glucose: Normal
- Renal function tests: Normal
- ECG: Normal preoperative evaluation
Diagnosis
Based on clinical examination and imaging findings, a diagnosis of: Macula-off rhegmatogenous retinal detachment of the left eye was established.
Management and Outcome
Treatment Strategy
The goals of management included:
- Closure of retinal tear
- Reattachment of the retina
- Prevention of recurrent detachment
- Restoration of visual function
Surgical Management
The patient underwent:
- Pars plana vitrectomy
- Fluid-air exchange
- Endolaser photocoagulation
- Intravitreal gas tamponade using sulfur hexafluoride (SF6)
Postoperative Care
- Topical antibiotic eye drops
- Topical corticosteroids
- Cycloplegic eye drops
- Strict prone positioning advised
- Avoidance of air travel
Clinical Course
Immediate Postoperative Period
- Retina successfully reattached
- Mild postoperative inflammation
- Intraocular pressure stable
Follow-Up
At 1 Week
- Retina attached
- Reduction in subretinal fluid
- Vision improving gradually
At 1 Month
- Visual acuity improved to 6/36
- Gas bubble partially absorbed
- No recurrent detachment
At 3 Months
- Retina remained attached
- Visual acuity improved to 6/18
- Significant subjective improvement reported
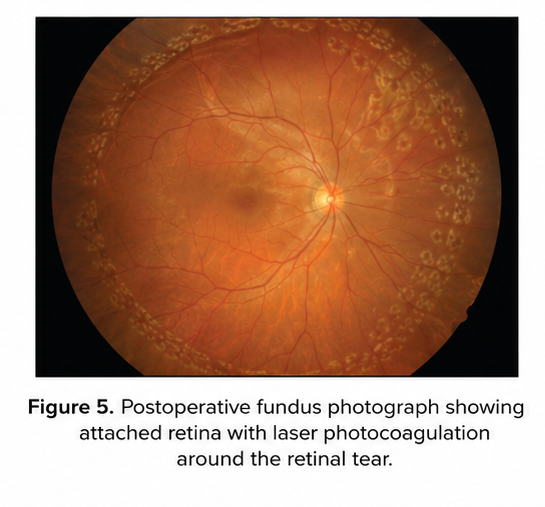
Discussion
Pathophysiology
Rhegmatogenous retinal detachment occurs when retinal breaks permit vitreous fluid to enter the subretinal space, causing separation of the neurosensory retina from the retinal pigment epithelium.
The underlying mechanisms include:
- Posterior vitreous detachment
- Vitreoretinal traction
- Retinal tear formation
- Subretinal fluid accumulation
Prolonged detachment leads to photoreceptor degeneration and permanent vision loss.
Risk Factors
Major risk factors include:
- High myopia
- Increasing age
- Cataract surgery
- Ocular trauma
- Family history
- Lattice degeneration
- Previous retinal detachment in fellow eye
In this patient, high myopia and prior cataract surgery likely contributed significantly.
Epidemiology
- Incidence: 10–18 per 100,000 population annually
- More common in males
- Peak incidence: 50–70 years
- Bilateral involvement possible
Retinal detachment remains one of the most common retinal emergencies worldwide.
Clinical Manifestations
Early Symptoms
- Flashes of light (photopsia)
- Floaters
- Blurred vision
Progressive Symptoms
- Peripheral visual field defects
- Curtain-like shadow
- Sudden visual loss
Signs
- Retinal elevation
- Retinal tears
- Vitreous pigment cells
- Reduced visual acuity
Macular involvement significantly worsens visual prognosis.
Diagnostic Considerations
Diagnosis primarily depends on:
- Detailed symptom history
- Dilated retinal examination
- Optical coherence tomography
- B-scan ultrasonography
Early diagnosis is critical because delayed treatment reduces visual recovery potential.
Treatment Modalities
Laser Photocoagulation
Used for:
- Small retinal tears
- Prophylaxis in high-risk lesions
Pneumatic Retinopexy
Suitable for selected superior retinal detachments.
Scleral Buckling
Traditionally used in younger patients with localized tears.
Pars Plana Vitrectomy
Currently preferred in:
- Complex detachments
- Pseudophakic eyes
- Macula-off detachments
This patient underwent vitrectomy due to macular involvement and pseudophakia.
Complications
Potential complications include:
- Recurrent retinal detachment
- Proliferative vitreoretinopathy
- Cataract formation
- Elevated intraocular pressure
- Epiretinal membrane formation
- Permanent visual impairment
Early surgical intervention significantly reduces complication rates.
Prognosis
The prognosis depends on:
- Duration of detachment
- Macular involvement
- Promptness of treatment
- Presence of proliferative vitreoretinopathy
Macula-on detachments generally have better outcomes compared to macula-off detachments.
In this case, timely surgery resulted in favorable anatomical and functional recovery.
Conclusion
Retinal detachment is a vision-threatening ophthalmologic emergency requiring immediate diagnosis and intervention. This case emphasizes the importance of recognizing warning symptoms such as flashes, floaters, and sudden visual field defects.
Comprehensive ophthalmic evaluation and prompt surgical management are crucial for preserving vision and preventing permanent blindness. Advances in vitreoretinal surgical techniques have significantly improved retinal reattachment success rates and visual outcomes.
Patient education regarding early symptoms and regular ophthalmologic follow-up in high-risk individuals remain essential components of preventive eye care.
References
- Mitry D, Charteris DG, Fleck BW, Campbell H, Singh J. The epidemiology of rhegmatogenous retinal detachment. https://pubmed.ncbi.nlm.nih.gov/19223912/
- Ghazi NG, Green WR. Pathology and pathogenesis of retinal detachment. https://pubmed.ncbi.nlm.nih.gov/16376651/
- American Academy of Ophthalmology. Retinal Detachment Preferred Practice Pattern. https://www.aao.org/
- Feltgen N, Walter P. Rhegmatogenous retinal detachment—an ophthalmologic emergency. https://pubmed.ncbi.nlm.nih.gov/21845416/
- Ross WH. Visual recovery after retinal detachment surgery. https://pubmed.ncbi.nlm.nih.gov/9818612/
- Schwartz SG, Flynn HW Jr. Pars plana vitrectomy for retinal detachment. https://pubmed.ncbi.nlm.nih.gov/24732768/
- National Eye Institute. Retinal Detachment Overview. https://www.nei.nih.gov/
Read more such content on @ Hidoc Dr | Medical Learning App for Doctors
Recommended News For You
Recommended Articles For You
Featured News
Featured Articles
Featured Events
Featured KOL Videos
1.
Parkinson patient's gait is restored by a spinal cord stimulator.
2.
EBCC: European Breast Cancer Conference
3.
The need for more Latinx participants in Alzheimer's trials is urgent.
4.
The most precise research tools for the deadliest blood cancer have been developed.
5.
CAR Natural Killer Cell Therapy Shows Promise in B-Cell Lymphomas
1.
The Lung Cancer Shift: From Reactive Treatment to Proactive Precision Medicine
2.
All You Need To Know About Melanoma Maligna: Causes, Symptoms & Treatment
3.
A Mural of Thrombus: Unlocking the Power of Art to Combat Cardiovascular Disease
4.
Hypercoagulable State: Factors that Contribute to Blood Clots
5.
Predicting Incidental Prostate Cancer in BPH Surgery Patients
1.
International Lung Cancer Congress®
2.
Genito-Urinary Oncology Summit 2026
3.
Future NRG Oncology Meeting
4.
ISMB 2026 (Intelligent Systems for Molecular Biology)
5.
Annual International Congress on the Future of Breast Cancer East
1.
Advances in Classification/ Risk Stratification of Plasma Cell Dyscrasias- The Summary
2.
Pazopanib: A Game-Changer in Managing Advanced Renal Cell Carcinoma
3.
Incidence of Lung Cancer- An Overview to Understand ALK Rearranged NSCLC
4.
Current Scenario of Cancer- An Overview of The Incidence of Cancer in Men
5.
Role of Nimotuzumab in Management of Nasopharyngeal Cancer
© Copyright 2026 Hidoc Dr. Inc.
Terms & Conditions - LLP | Inc. | Privacy Policy - LLP | Inc. | Account Deactivation

