Herpes Zoster: Clinical Presentation, Diagnostic Evaluation, Management, and Outcomes - A Case Report
OthersPage Navigation
Abstract
Herpes zoster is a neurocutaneous viral infection caused by reactivation of latent varicella-zoster virus (VZV) within dorsal root ganglia, presenting as a painful, unilateral vesicular rash in a dermatomal distribution. The condition is associated with acute neuritic pain and may lead to significant morbidity, particularly postherpetic neuralgia (PHN), especially in older adults and immunocompromised individuals. Early recognition and prompt antiviral therapy are critical in reducing symptom severity, viral shedding, and the risk of complications. We report a case of a middle-aged male presenting with severe unilateral thoracic pain followed by a vesicular rash consistent with herpes zoster. This case highlights clinical presentation, diagnostic evaluation, antiviral and supportive management, pain control strategies, and short-term outcomes. The report emphasizes the importance of early antiviral initiation, adequate analgesia, complication prevention, and vaccination counseling to reduce disease burden and recurrence.
Introduction
Herpes zoster results from reactivation of latent varicella-zoster virus following primary varicella infection, typically decades later. Reactivation occurs due to decline in cell-mediated immunity, commonly associated with aging, diabetes mellitus, malignancy, immunosuppressive therapy, or psychological stress. The incidence of herpes zoster increases with advancing age and comorbid conditions. Commonly affected dermatomes include thoracic, cranial (trigeminal), and lumbar regions. Complications include postherpetic neuralgia, secondary bacterial infection, ocular involvement (herpes zoster ophthalmicus), and, rarely, neurological complications such as meningitis or encephalitis. Early diagnosis and initiation of antiviral therapy within 72 hours of rash onset significantly improves outcomes and reduces complications.
Case Report
Patient History
A 56-year-old male with a history of type 2 diabetes mellitus and dyslipidemia presented to the outpatient clinic with a 3-day history of severe burning pain over the right chest wall, followed by the appearance of a painful, blistering rash. The pain was described as sharp, electric shock-like, and worsened by touch and clothing contact. There was no history of recent trauma, fever, or similar past episodes. The patient had a history of childhood chickenpox and had not received herpes zoster vaccination.
Clinical Examination
On examination, the patient was afebrile and hemodynamically stable. Dermatological evaluation revealed multiple grouped vesicles on an erythematous base distributed along the right T6–T7 dermatome, not crossing the midline.
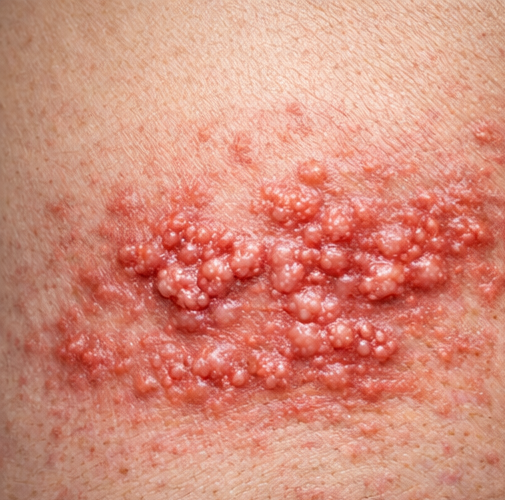
The lesions were tender to palpation with surrounding hyperesthesia. No ocular or facial involvement was noted. Neurological examination was otherwise unremarkable.
Clinical Evaluation
Differential Diagnosis
• Herpes zoster (shingles)
• Contact dermatitis
• Herpes simplex virus infection
• Impetigo
• Allergic drug eruption
Investigations
The diagnosis was primarily clinical based on the characteristic dermatomal vesicular rash and neuropathic pain.
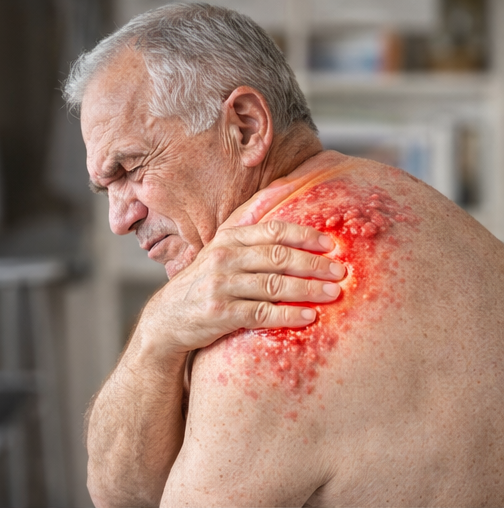
Baseline laboratory investigations, including complete blood count and blood glucose levels, were within acceptable limits except for suboptimal glycemic control (HbA1c 8.4%). No evidence of secondary bacterial infection was present. Virological confirmation by polymerase chain reaction (PCR) for VZV from vesicular fluid was not deemed necessary due to typical clinical features.
Management and Outcome
Management Strategy
Antiviral therapy was initiated within 72 hours of rash onset using oral valacyclovir (1 g three times daily for 7 days).
Adequate analgesia was provided using a stepwise approach, including paracetamol and gabapentin for neuropathic pain. Topical calamine lotion and cool compresses were advised for symptomatic relief. The patient was counseled regarding skin hygiene to prevent secondary bacterial infection and advised to avoid contact with pregnant women, neonates, and immunocompromised individuals until lesion crusting occurred.

Glycemic control was optimized with adjustment of antidiabetic therapy.
The patient was educated regarding early signs of complications and advised to return for worsening pain, fever, or spread of lesions.
Follow-Up and Outcome
At 10-day follow-up, the vesicular lesions had crusted and were healing well, with significant reduction in erythema and pain intensity. The patient reported residual mild neuropathic discomfort, managed with continued low-dose gabapentin. At 4-week follow-up, the skin lesions had resolved completely with minimal residual hyperpigmentation and no features of postherpetic neuralgia. The patient was counseled regarding herpes zoster vaccination for prevention of recurrence and reduction of PHN risk.
Discussion
Herpes zoster results from reactivation of latent VZV due to waning cell-mediated immunity. Prodromal neuropathic pain often precedes the rash and can lead to diagnostic delay. Early antiviral therapy within 72 hours of rash onset reduces viral replication, accelerates lesion healing, shortens duration of acute pain, and decreases the risk of PHN. Valacyclovir and famciclovir offer improved bioavailability and dosing convenience compared to acyclovir.
Adequate pain control is central to management, as uncontrolled acute zoster pain is a major risk factor for PHN. Neuropathic agents such as gabapentin or pregabalin may be required in addition to simple analgesics. Complications such as herpes zoster ophthalmicus require urgent ophthalmology referral due to risk of vision loss. Vaccination with recombinant zoster vaccine is effective in reducing herpes zoster incidence and PHN, particularly in adults aged ≥50 years and high-risk individuals.
Conclusion
Herpes zoster is a common neurocutaneous infection associated with significant morbidity, particularly among older adults and individuals with comorbidities such as diabetes mellitus, malignancy, and immunosuppressive conditions. The disease burden extends beyond the acute vesicular eruption to include substantial functional impairment, reduced quality of life, and healthcare utilization. Early clinical recognition and prompt initiation of antiviral therapy within the recommended therapeutic window are essential to improve clinical outcomes, shorten disease duration, and reduce the risk of complications, including postherpetic neuralgia and secondary bacterial infection.
Comprehensive management requires effective multimodal pain control, prevention and early treatment of secondary skin infections, optimization of underlying comorbid conditions, and patient education regarding transmission risk and complication warning signs. Vaccination remains a key preventive strategy, with recombinant zoster vaccines demonstrating high efficacy in reducing disease incidence, severity, recurrence, and long-term sequelae such as postherpetic neuralgia, thereby significantly lowering overall disease burden.
References
- Cohen JI. Herpes zoster. N Engl J Med. 2013;369(3):255–263.
- Dworkin RH, Johnson RW, Breuer J, et al. Recommendations for the management of herpes zoster. Clin Infect Dis. 2007;44(Suppl 1):S1–S26.
- Koshy E, Mengting L, Kumar H, Jianbo W. Epidemiology, treatment, and prevention of herpes zoster: A comprehensive review. Indian J Dermatol Venereol Leprol. 2018;84(3):251–262.
- Cunningham AL, Lal H, Kovac M, et al. Efficacy of the herpes zoster subunit vaccine in older adults. N Engl J Med. 2015;372:2087–2096.
- Oxman MN, Levin MJ, Johnson GR, et al. A vaccine to prevent herpes zoster and postherpetic neuralgia in older adults. N Engl J Med. 2005;352:2271–2284.
Read more such content on @ Hidoc Dr | Medical Learning App for Doctors
Recommended News For You
Recommended Articles For You
Featured News
Featured Articles
Featured Events
Featured KOL Videos
1.
Researchers find distinct cell receptors with the potential for new treatments.
2.
Breast cancer patients' arms swell less after an effective lymph node transfer.
3.
Telehealth in the pandemic era resulted in fewer therapy interruptions.
4.
Too Many Chest CTs for Incidental Lung Nodules?
5.
Global warming could be driving up women's cancer risk, find researchers
1.
The New Frontier of Cancer Survivorship: Navigating the Long-Term Effects of Immunotherapy and Targeted Therapies
2.
Deterministic Reprogramming of Neutrophils within Tumors: A New Frontier in Cancer Research
3.
Neuroendocrine Tumors: Case Study on Diagnosis, Treatment Strategies & Patient Management
4.
Ticagrelor Monotherapy vs. Ticagrelor + Aspirin in ACS Post-PCI: ULTIMATE-DAPT Trial
5.
Transfusing the Future: Exploring the Possibilities of Blood Transfusions
1.
International Lung Cancer Congress®
2.
Genito-Urinary Oncology Summit 2026
3.
Future NRG Oncology Meeting
4.
ISMB 2026 (Intelligent Systems for Molecular Biology)
5.
Annual International Congress on the Future of Breast Cancer East
1.
Current Scenario of Blood Cancer- A Conclusion on Genomic Testing & Advancement in Diagnosis and Treatment
2.
Navigating the Brain Barrier: The CNS Challenge in ALK+ NSCLC
3.
Thromboprophylaxis In Medical Settings
4.
Treatment Paradigm for Patients with R/R Adult B-cell ALL- Expert Discussions
5.
Current Scenario of Blood Cancer- Genomic Testing & Advancement in Diagnosis and Treatment
© Copyright 2026 Hidoc Dr. Inc.
Terms & Conditions - LLP | Inc. | Privacy Policy - LLP | Inc. | Account Deactivation

