Degloving Injury: Clinical Presentation, Diagnostic Evaluation, Management, and Outcomes – A Case Report
OthersPage Navigation
Abstract
Degloving injuries are severe traumatic soft-tissue injuries characterized by the avulsion of skin and subcutaneous tissue from the underlying fascia, muscle, or bone, resulting in disruption of blood supply and extensive tissue damage. These injuries most commonly occur following high-energy trauma such as road traffic accidents, industrial accidents, or crush injuries. Degloving injuries are associated with significant morbidity due to risks of infection, tissue necrosis, functional impairment, and prolonged hospitalization. Clinical presentation varies depending on the mechanism and extent of injury and may range from partial skin avulsion to extensive circumferential soft-tissue loss. Early recognition, prompt diagnostic evaluation, and a multidisciplinary management approach are critical for limb salvage and optimal functional outcomes. Diagnosis is primarily clinical, supported by imaging to assess soft-tissue viability, associated fractures, and vascular involvement. Management strategies include early wound stabilization, surgical debridement, soft-tissue reconstruction, infection control, and rehabilitation. This case report describes an adult patient with a lower-limb degloving injury following a road traffic accident, highlighting clinical features, diagnostic workup, management approach, and short-term outcomes.
Introduction
Degloving injuries represent a complex form of traumatic soft-tissue injury resulting from tangential or shearing forces that separate the skin and subcutaneous tissues from deeper structures. This separation disrupts perforating vessels, leading to compromised tissue perfusion and a high risk of necrosis. Degloving injuries can be classified as open or closed, with open injuries presenting with visible avulsion and closed injuries, such as Morel-Lavallée lesions, presenting with internal degloving and hematoma formation.
These injuries are most frequently encountered in high-velocity trauma, including road traffic accidents, agricultural and industrial injuries, and crush mechanisms. Lower limbs are commonly affected, particularly the thigh, leg, and foot, though upper limbs, trunk, and scalp may also be involved. Degloving injuries pose significant challenges due to their extensive surface area, contamination, and associated injuries such as fractures, vascular compromise, and nerve damage.
Early diagnosis and timely intervention are essential to prevent complications such as infection, tissue loss, delayed wound healing, and long-term functional disability. A multidisciplinary approach involving trauma surgeons, orthopedic surgeons, plastic surgeons, radiologists, nurses, and physiotherapists is often required. This case report illustrates the clinical course and management of a lower-limb degloving injury in a hospitalized adult patient.
Case Report
Patient History
A 38-year-old male was brought to the emergency department following a high-speed road traffic accident involving a motorcycle collision with a heavy vehicle. The patient was conscious at presentation and complained of severe pain and bleeding from the left lower limb. There was no history of loss of consciousness.
The patient had no known chronic medical illnesses and no prior history of trauma or surgery. He was a non-smoker and reported no regular medication use.
Clinical Examination
On initial assessment, the patient was hemodynamically stable, with a blood pressure of 118/74 mmHg, heart rate of 96 beats per minute, and oxygen saturation of 98% on room air. Primary trauma survey revealed no airway or breathing compromise.
Local examination of the left lower limb demonstrated an extensive open degloving injury involving the anteromedial aspect of the leg, extending from the proximal tibia to the ankle.
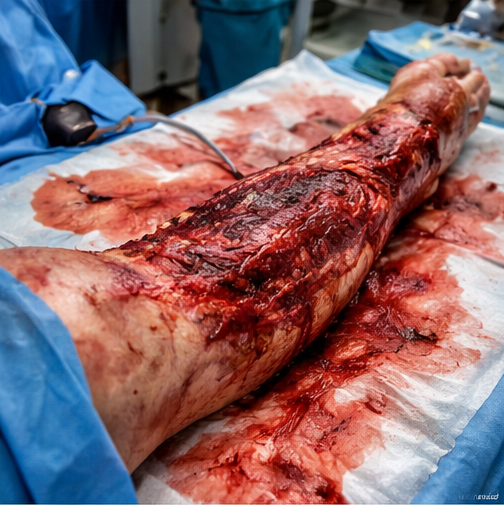
The skin and subcutaneous tissue were avulsed, exposing underlying fascia and muscle. The wound was contaminated with road debris and showed irregular wound margins with areas of dusky, nonviable skin. Active bleeding was present but controlled with compression.
Distal pulses (dorsalis pedis and posterior tibial) were palpable, and capillary refill time was less than two seconds. Sensory and motor function of the foot were preserved.
Clinical Evaluation
Differential Diagnosis
The differential diagnosis included:
- Open degloving injury
- Extensive laceration with skin loss
- Crush injury with soft-tissue necrosis
- Open fracture with soft-tissue compromise
The mechanism of injury, clinical appearance, and circumferential avulsion strongly supported a diagnosis of an open degloving injury.
Investigations
- Laboratory tests: Mild anemia; leukocyte count within normal limits; renal and liver function tests normal
- Imaging:
- X-ray of the left leg: No associated fractures
- Doppler ultrasound: Patent arterial flow with no evidence of vascular injury
- Microbiological evaluation: Wound swab collected intraoperatively for culture
Advanced imaging was deferred initially due to clear clinical findings and preserved distal perfusion.
Management and Outcome
Initial Management
Immediate management followed trauma care principles:
- Wound irrigation with copious normal saline
- Sterile dressing and limb immobilization
- Intravenous broad-spectrum antibiotics initiated
- Tetanus prophylaxis administered
- Adequate analgesia provided
The patient was taken to the operating theater within six hours of injury for surgical exploration.
Surgical Management
Under regional anesthesia, thorough wound exploration was performed.
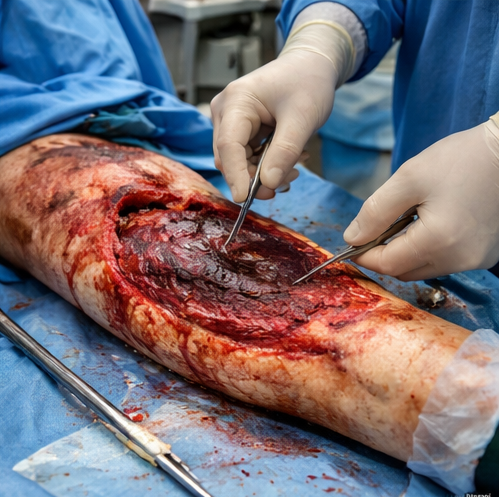
Devitalized skin and subcutaneous tissue were excised, and the wound was extensively irrigated. Marginally viable skin flaps were preserved where possible. No muscle necrosis or vascular injury was identified.
Given the extent of soft-tissue loss and contamination, primary closure was not feasible. Negative pressure wound therapy (NPWT) was applied to promote granulation tissue formation and reduce wound edema.
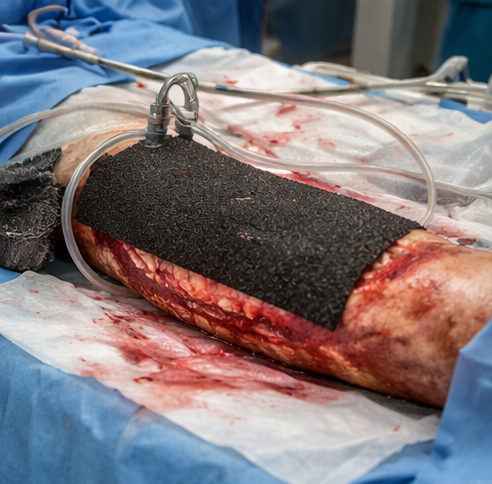
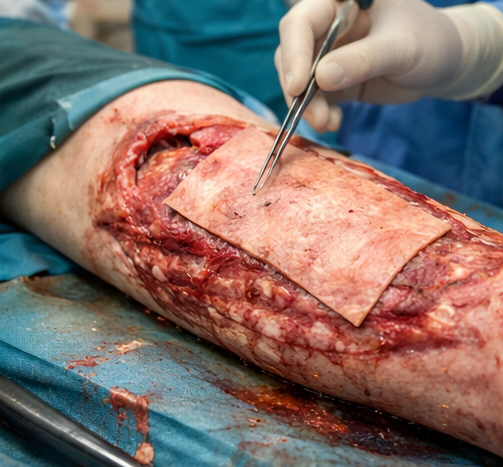
Definitive Wound Management
Serial debridements were performed over the next week. Once a healthy granulation bed was achieved, split-thickness skin grafting was performed using a donor site from the contralateral thigh. The graft was secured, and NPWT was reapplied to enhance graft adherence.
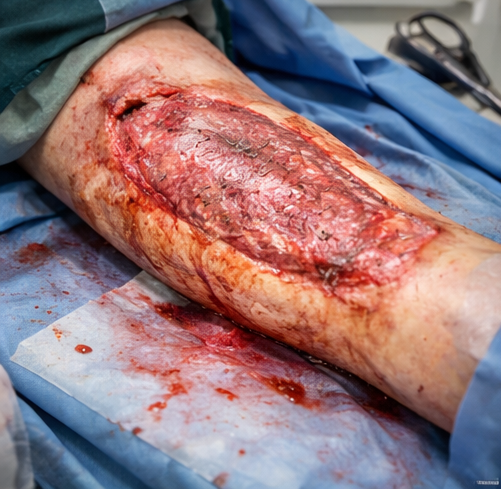
Follow-Up and Outcome
At two-week follow-up, the skin graft demonstrated good uptake with minimal areas of graft loss. There were no signs of infection or wound breakdown. The patient was started on gradual weight-bearing and physiotherapy to maintain joint mobility and muscle strength.
At six weeks, complete wound healing was achieved with satisfactory cosmetic and functional outcomes. The patient regained full ambulation with minimal residual stiffness and returned to daily activities.
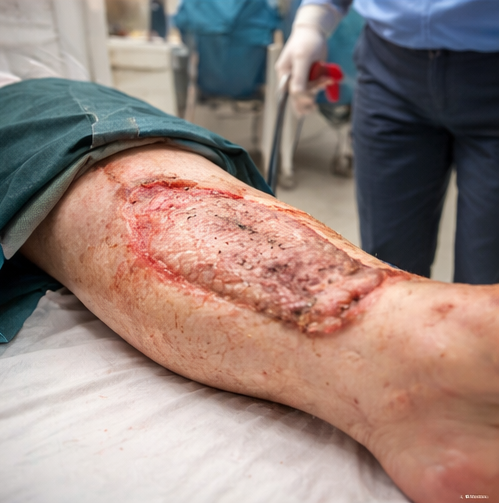
Discussion
Degloving injuries are among the most challenging soft-tissue injuries encountered in trauma care due to their complexity and high risk of complications. The shearing mechanism leads to disruption of perforating vessels, making assessment of tissue viability difficult at initial presentation. Clinical judgment remains the cornerstone of diagnosis, supplemented by imaging when vascular or deep tissue involvement is suspected.
Early and aggressive debridement is essential to prevent infection and promote healing. Delayed recognition or inadequate initial management can result in extensive tissue necrosis, sepsis, and limb loss. NPWT has become an important adjunct in managing degloving injuries by promoting granulation tissue formation and preparing the wound bed for definitive reconstruction.
Reconstruction options depend on the extent and location of injury and may include skin grafts, local flaps, or free tissue transfer. Rehabilitation plays a crucial role in restoring function and preventing long-term disability.
This case demonstrates that timely surgical intervention, meticulous wound care, and a multidisciplinary approach can result in favorable outcomes even in extensive degloving injuries.
Conclusion
Degloving injuries are severe traumatic soft-tissue injuries associated with significant morbidity if not promptly and appropriately managed. Early diagnosis, aggressive debridement, appropriate wound coverage, and structured rehabilitation are key determinants of successful outcomes. A multidisciplinary approach is essential to minimize complications, preserve limb function, and improve patient quality of life.
References
- Hudson, D. A. (1996). Missed closed degloving injuries: Late presentation with chronic seromas. British Journal of Plastic Surgery, 49(3), 145–147. https://pubmed.ncbi.nlm.nih.gov/8736538/
- Hak, D. J., Olson, S. A., & Matta, J. M. (1997). Diagnosis and management of closed internal degloving injuries associated with pelvic and acetabular fractures. Journal of Trauma, 42(6), 1046–1051. https://pubmed.ncbi.nlm.nih.gov/9210535/
- Tejwani, S. G., Cohen, S. B., & Bradley, J. P. (2007). Management of Morel-Lavallée lesion of the knee: Twenty-seven cases in the National Football League. American Journal of Sports Medicine, 35(7), 1162–1167. https://pubmed.ncbi.nlm.nih.gov/17426382/
- Hudson, D. A., Knottenbelt, J. D., & Krige, J. E. (1992). Closed degloving injuries: Results following conservative surgery. Plastic and Reconstructive Surgery, 89(5), 853–855 https://pubmed.ncbi.nlm.nih.gov/1562225
Read more such content on @ Hidoc Dr | Medical Learning App for Doctors
Recommended News For You
Recommended Articles For You
Featured News
Featured Articles
Featured Events
Featured KOL Videos
1.
Nuclear missile workers are contracting cancer: They blame the bases
2.
Mixed Results With Cyclophosphamide in Mismatched Unrelated Stem Cell Transplants
3.
New analysis helps discern benign from malignant thyroid growths
4.
MCh in Gynecologic Oncology: Admission, Medical School, Fees, Qualifications Information
5.
Even a few mutated cells can significantly impact how blood cancers develop, study finds
1.
Uncovering the Hidden Signs: How to Recognize the Early Symptoms of Colon Cancer
2.
The benefits and risks of taking fludrocortisone for adrenal insufficiency
3.
IGSF8: A Rising Star in Cancer Immunotherapy - Harnessing the Innate Immune System
4.
Innovative Intraoperative Therapies in Neurosurgical Oncology: Advancing Precision and Outcomes
5.
Different Types of Blood Dyscrasias
1.
International Lung Cancer Congress®
2.
Genito-Urinary Oncology Summit 2026
3.
Future NRG Oncology Meeting
4.
ISMB 2026 (Intelligent Systems for Molecular Biology)
5.
Annual International Congress on the Future of Breast Cancer East
1.
An In-Depth Look At The Signs And Symptoms Of Lymphoma
2.
Iron Deficiency Anemia: Ferric Maltol As a New Treatment Option- Further Discussion on A New Perspective
3.
Revolutionizing Treatment of ALK Rearranged NSCLC with Lorlatinib - Part VII
4.
Virtual Case Study on Pedal Edema and Triple Vessel Disease - An Initiative by Hidoc Dr.
5.
Nimotozumab Plus Chemo-radiotherapy v/s Placebo Plus Chemo-radiotherapy in Locally Advanced Nasopharyngeal Carcinoma
© Copyright 2026 Hidoc Dr. Inc.
Terms & Conditions - LLP | Inc. | Privacy Policy - LLP | Inc. | Account Deactivation

