Comedones: Clinical Presentation, Diagnostic Evaluation, Management, and Outcomes – A Case Report
OthersPage Navigation
Abstract
Comedones are non-inflammatory acne lesions that result from obstruction of the pilosebaceous unit due to abnormal keratinization and increased sebum production. They represent the earliest manifestation of acne vulgaris and are classified into open comedones (blackheads) and closed comedones (whiteheads). Although commonly seen during adolescence, comedonal acne may persist into adulthood and significantly affect cosmetic appearance and psychological well-being.
We present the case of a 19-year-old female who presented with multiple facial blackheads and whiteheads predominantly involving the forehead, nose, and cheeks for 1 year. The lesions gradually increased in number and were associated with oily skin and occasional mild inflammatory papules. Dermatological examination confirmed multiple open and closed comedones without significant nodulocystic lesions. The patient was diagnosed with comedonal acne and managed with topical retinoids, skin care modification, and lifestyle counseling, resulting in significant clinical improvement.
This case highlights the importance of early diagnosis and appropriate management of comedonal acne to prevent progression to inflammatory acne and reduce long-term cosmetic complications.
Introduction
Comedones are the hallmark lesions of acne vulgaris and develop due to blockage of hair follicles by keratin, sebum, and cellular debris. They are among the most common dermatological conditions affecting adolescents and young adults.
Comedones are classified into:
• Open comedones (blackheads)
• Closed comedones (whiteheads)
Open comedones appear as dark-colored follicular plugs due to oxidation of melanin and lipids on exposure to air, whereas closed comedones appear as small flesh-colored or white papules covered by epidermis.
The pathogenesis involves multiple factors including:
• Increased sebum production
• Follicular hyperkeratinization
• Cutibacterium acnes colonization
• Hormonal influences
• Inflammatory mediators
Commonly affected areas include:
• Face
• Forehead
• Nose
• Chin
• Upper chest
• Back
Comedonal acne may worsen due to cosmetic products, hormonal fluctuations, stress, excessive humidity, and poor skin hygiene practices.
Acne vulgaris affects approximately 80–90% of adolescents worldwide and can significantly impact self-esteem, emotional health, and social interactions.
Early treatment is important to prevent inflammatory transformation, post-inflammatory hyperpigmentation, and acne scarring.
Case Report
Patient History
A 19-year-old female presented to the dermatology outpatient department with:
• Multiple blackheads and whiteheads over the face for 1 year
• Gradual increase in lesions over the forehead, nose, and cheeks
• Oily skin with occasional acne flare-ups
• Mild cosmetic concern and reduced self-confidence
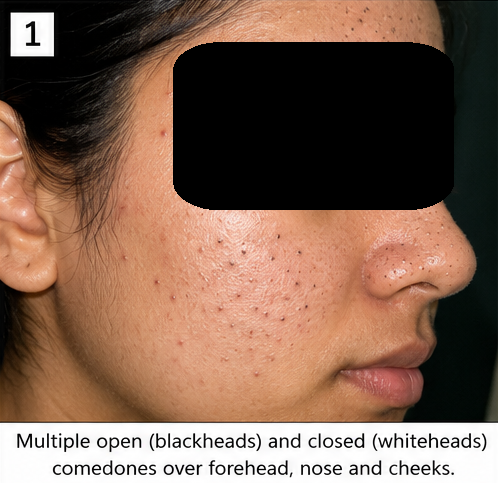
The patient denied:
• Painful nodules
• Pus discharge
• Fever
• Itching
• Drug intake associated with acne
• Menstrual irregularities
Medical history revealed:
• No diabetes mellitus
• No endocrine disorders
• No previous dermatological illness
Family history showed mild acne in the patient’s mother during adolescence.
Clinical Examination
General Examination
• Patient conscious and cooperative
• Vitals stable
• Afebrile
• No systemic abnormalities detected
Dermatological Examination
Examination of the face revealed:
• Multiple open comedones over the nose and cheeks
• Numerous closed comedones over the forehead and chin
• Mild seborrhea
• Few inflammatory papules
• No nodules or cysts
• No scarring
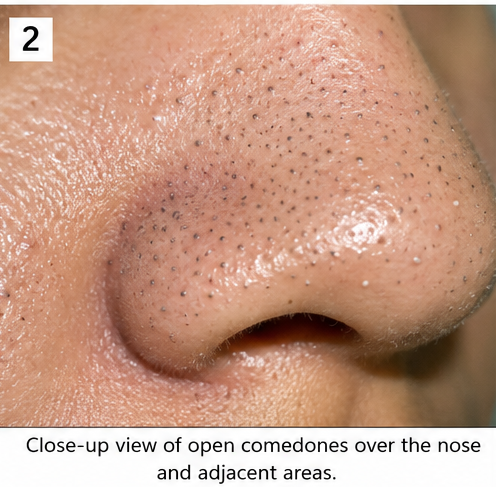
Skin over the chest and back showed minimal involvement.
Hair and nail examination were normal.
Clinical Evaluation
Differential Diagnosis
Based on clinical presentation, the following conditions were considered:
• Comedonal acne
• Milia
• Sebaceous hyperplasia
• Folliculitis
• Acne cosmetica
• Perioral dermatitis
The characteristic presence of open and closed comedones strongly suggested comedonal acne.
Investigations
Routine Laboratory Tests
• Complete blood count: Normal
• Blood glucose levels: Normal
• Thyroid profile: Normal
Hormonal Evaluation
Not indicated due to absence of signs suggestive of hormonal imbalance.
Dermoscopic Examination
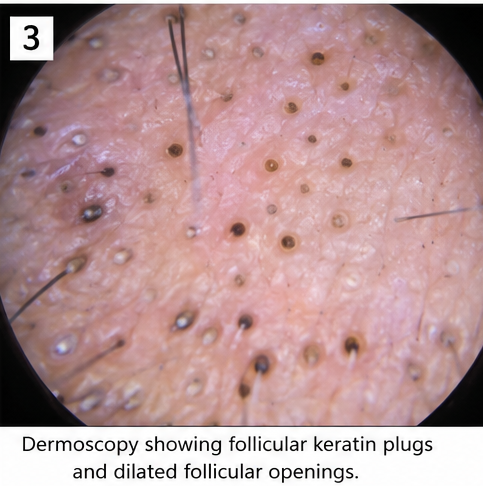
Findings included:
• Follicular keratin plugs
• Dilated follicular openings
• Increased sebaceous activity
Diagnosis
Based on clinical examination, the diagnosis of:
Mild to Moderate Comedonal Acne (Acne Vulgaris)
was established.
Management and Outcome
Treatment Strategy
The goals of treatment included:
• Reduction of comedone formation
• Control of sebum production
• Prevention of inflammatory acne
• Improvement in cosmetic appearance
• Prevention of acne scarring
Medical Management
The patient was started on:
• Topical adapalene 0.1% gel at night
• Salicylic acid face wash
• Oil-free moisturizer
• Sunscreen application
• Lifestyle and dietary counseling

Patient education included:
• Avoid excessive face touching
• Avoid comedogenic cosmetic products
• Gentle cleansing twice daily
• Avoid squeezing lesions
Clinical Course
At 2 Weeks
• Mild skin dryness noted
• Reduction in new comedone formation
• Improved skin texture
At 6 Weeks
• Significant reduction in blackheads and whiteheads
• Decreased facial oiliness
• Better cosmetic appearance
At 3 Months
• Marked improvement in facial lesions
• Minimal residual comedones
• No inflammatory progression
• Improved self-confidence and quality of life
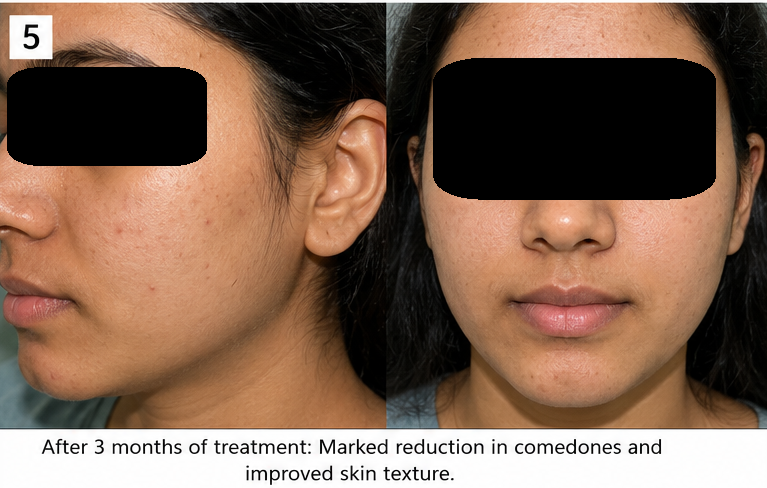
Discussion
Pathophysiology
Comedones develop due to obstruction of pilosebaceous follicles caused by abnormal keratinocyte shedding and excessive sebum accumulation.
Major pathogenic mechanisms include:
• Follicular hyperkeratinization
• Increased androgen-mediated sebum production
• Colonization by Cutibacterium acnes
• Local inflammatory responses
Closed comedones occur when follicular openings remain obstructed, while open comedones develop when follicular contents are exposed to air, leading to oxidation and dark discoloration.
Epidemiology
• Acne affects approximately 80–90% of adolescents
• Comedonal acne is the earliest form of acne vulgaris
• More common during puberty
• Increased prevalence in oily skin types
• May persist into adulthood
Clinical Manifestations
Typical Features
• Blackheads (open comedones)
• Whiteheads (closed comedones)
• Oily skin
• Mild inflammatory papules
Commonly Affected Sites
• Forehead
• Nose
• Chin
• Cheeks
• Upper back
• Chest
Aggravating Factors
• Hormonal changes
• Stress
• Oily cosmetics
• Humidity
• High glycemic diet
• Poor skin care practices
Diagnostic Considerations
Diagnosis is primarily clinical.
Important diagnostic components include:
- Detailed dermatological history
- Physical examination
- Assessment of acne severity
- Identification of triggering factors
- Exclusion of hormonal disorders when indicated
Dermoscopy may help visualize follicular plugs and sebaceous activity.
Treatment Modalities
Topical Therapy
First-line treatments include:
• Topical retinoids
• Adapalene
• Tretinoin
• Salicylic acid
• Benzoyl peroxide
Systemic Therapy
Indicated in moderate to severe acne:
• Oral antibiotics
• Hormonal therapy
• Oral isotretinoin
Procedural Treatments
In selected cases:
• Comedone extraction
• Chemical peels
• Laser therapy
• Microdermabrasion
Complications
Potential complications include:
• Inflammatory acne progression
• Post-inflammatory hyperpigmentation
• Acne scars
• Psychological distress
• Reduced self-esteem
Untreated acne may significantly affect social and emotional well-being.
Prognosis
The prognosis is generally favorable with early treatment and proper skin care.
Factors influencing prognosis include:
• Severity of acne
• Treatment adherence
• Hormonal influences
• Skin type
• Presence of inflammatory lesions
Most patients respond well to topical retinoid therapy and lifestyle modifications.
In this case, early dermatological intervention resulted in substantial clinical improvement and prevention of disease progression.
Conclusion
Comedones are the primary lesions of acne vulgaris and represent an important early stage in acne development. Early recognition and treatment are essential to prevent inflammatory progression, pigmentation, and scarring.
This case highlights the importance of appropriate dermatological evaluation, patient education, and adherence to topical therapy in achieving favorable outcomes.
Comprehensive management involving medical treatment, skin care optimization, and lifestyle modification remains the cornerstone of successful comedonal acne treatment.
References
- Thiboutot D, Gollnick H, Bettoli V, et al. New insights into the management of acne. https://pubmed.ncbi.nlm.nih.gov/20920852/
- Zaenglein AL, Pathy AL, Schlosser BJ, et al. Guidelines of care for the management of acne vulgaris. https://pubmed.ncbi.nlm.nih.gov/26897386/
- Titus S, Hodge J. Diagnosis and treatment of acne. https://pubmed.ncbi.nlm.nih.gov/25591226/
- Webster GF. Acne vulgaris. https://pubmed.ncbi.nlm.nih.gov/21824505/
- Williams HC, Dellavalle RP, Garner S. Acne vulgaris. https://pubmed.ncbi.nlm.nih.gov/21880356/
- American Academy of Dermatology. Acne: Diagnosis and treatment. American Academy of Dermatology
- National Institute of Arthritis and Musculoskeletal and Skin Diseases. Acne Overview. NIAMS Acne Information
Read more such content on @ Hidoc Dr | Medical Learning App for Doctors
Recommended News For You
Recommended Articles For You
Featured News
Featured Articles
Featured Events
Featured KOL Videos
1.
Reducing social media to an hour a day boosts young people's self-image.
2.
ICIs Show High Responses in Mediastinal B-Cell Lymphoma
3.
Modified personalized cancer vaccine generates powerful immune response
4.
In Acute Leukemia With Heavily Pretreated Patients, Menin Inhibitor Yields 63 Percent ORR.
5.
After three years, responses to mounetuzumab in follicular lymphoma are still stable.
1.
Empowering Lung Cancer Diagnosis Through the Synergy of Advanced Technologies and Artificial Intelligence
2.
Revolutionizing Oncology: AI in Radiology, Machine Learning in Pathology, and Deep Learning for Cancer Detection
3.
Emerging Therapies and Technologies Reshaping Oncology: Innovations and Impact in 2025
4.
Can We Repurpose BV-CHP for Better Outcomes in Peripheral T-Cell Lymphoma?
5.
Understanding Bone Metastases: How Long Can Someone Live When Cancer Spreads To The Bones?
1.
International Lung Cancer Congress®
2.
Genito-Urinary Oncology Summit 2026
3.
Future NRG Oncology Meeting
4.
ISMB 2026 (Intelligent Systems for Molecular Biology)
5.
Annual International Congress on the Future of Breast Cancer East
1.
Untangling The Best Treatment Approaches For ALK Positive Lung Cancer - Part VIII
2.
Efficient Management of First line ALK-rearranged NSCLC - Part VI
3.
The Era of Targeted Therapies for ALK+ NSCLC: A Paradigm Shift
4.
Efficient Management of First line ALK-rearranged NSCLC - Part VII
5.
Pazopanib Takes Center Stage in Managing Renal Cell Carcinoma - Part III
© Copyright 2026 Hidoc Dr. Inc.
Terms & Conditions - LLP | Inc. | Privacy Policy - LLP | Inc. | Account Deactivation

