Scalp Psoriasis: Clinical Presentation, Diagnostic Evaluation, Management, and Outcomes – A Case Report
OthersPage Navigation
Abstract
Scalp psoriasis is a chronic, immune-mediated inflammatory dermatological disorder characterized by erythematous plaques covered with silvery-white scales involving the scalp. It represents one of the most common manifestations of psoriasis and can significantly impair quality of life due to persistent itching, visible scaling, discomfort, and psychosocial distress. Although scalp psoriasis is not life-threatening, severe and untreated disease may lead to secondary infections, temporary hair shedding, sleep disturbances, and emotional stress.
We report the case of a 42-year-old male presenting with persistent scalp scaling, intense pruritus, and progressive erythematous plaques over the scalp for approximately 1 year. Clinical examination and dermoscopic findings were suggestive of scalp psoriasis. The patient was managed with topical corticosteroids, keratolytic agents, vitamin D analogues, and lifestyle modifications, resulting in marked clinical improvement over subsequent follow-up visits.
This case highlights the importance of early recognition, accurate diagnosis, patient education, and long-term management strategies in achieving symptom control and improving quality of life in patients with scalp psoriasis.
Introduction
Psoriasis is a chronic inflammatory skin disorder characterized by hyperproliferation of keratinocytes and dysregulated immune activity. Scalp involvement occurs in nearly 50–80% of psoriasis patients and may occur either as an isolated manifestation or as part of generalized plaque psoriasis.
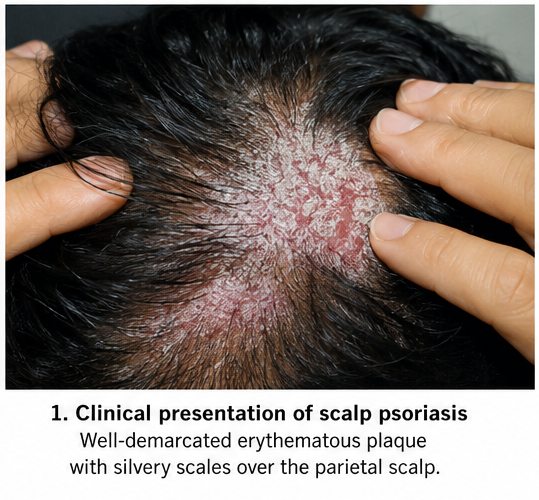
Scalp psoriasis commonly presents with sharply demarcated erythematous plaques covered by thick silvery scales. The lesions may extend beyond the hairline and are frequently associated with itching, burning sensation, irritation, and cosmetic embarrassment. In severe cases, extensive scaling and inflammation may contribute to temporary hair loss due to excessive scratching and inflammation.
The disease results from complex interactions between genetic predisposition, environmental triggers, and immune dysregulation involving T lymphocytes and inflammatory cytokines such as tumor necrosis factor-alpha (TNF-α), interleukin-17 (IL-17), and interleukin-23 (IL-23).
Although scalp psoriasis is not contagious, it can significantly affect emotional well-being, self-esteem, and social functioning. Advances in dermatologic therapies, including biologics and targeted immunomodulatory agents, have improved disease control and patient outcomes considerably.
Case Report
Patient History
A 42-year-old male presented to the dermatology outpatient department with the following complaints:
- Persistent itching over the scalp for 1 year
- Progressive flaky white scaling
- Red raised lesions over the scalp
- Occasional burning sensation
- Increased hair shedding during combing
The symptoms initially appeared as mild dandruff-like scaling over the occipital region and gradually progressed to involve the parietal and frontal scalp areas. The patient reported worsening itching during periods of stress and winter months.
There was no history of fever, weight loss, joint pain, or recent infections. The patient denied use of any new hair products or medications before symptom onset.
Past medical history revealed intermittent mild plaque psoriasis over the elbows several years earlier. Family history was significant for psoriasis in the patient’s father.
Clinical Examination
General Examination
- Patient conscious and oriented
- Vitals stable
- No pallor, cyanosis, or edema
Dermatological Examination
- Well-demarcated erythematous plaques over the scalp
- Thick silvery-white adherent scales present
- Lesions predominantly involving:
- Occipital region
- Parietal scalp
- Frontal hairline
- Mild excoriation marks due to scratching
- Minimal temporary diffuse hair thinning noted
- No pustules or secondary infection
Nail Examination
- Mild nail pitting observed
Joint Examination
- No evidence of psoriatic arthritis
Clinical Evaluation
Differential Diagnosis
Based on the clinical presentation, the following conditions were considered:
- Scalp psoriasis (most likely)
- Seborrheic dermatitis
- Tinea capitis
- Atopic dermatitis
- Discoid lupus erythematosus
The presence of sharply demarcated plaques with thick silvery scaling and positive family history strongly favored scalp psoriasis.
Investigations
Dermoscopy
Dermoscopic examination revealed:
- Red dotted vessels
- Diffuse white scaling
- Uniform vascular pattern
- Erythematous background
These findings were consistent with psoriasis.

Laboratory Investigations
- Complete blood count: Within normal limits
- Liver function tests: Normal
- Renal function tests: Normal
- ESR and CRP: Mildly elevated
- Fungal scraping (KOH mount): Negative
Skin Biopsy
Histopathological examination demonstrated:
- Hyperkeratosis
- Parakeratosis
- Acanthosis
- Elongation of rete ridges
- Munro microabscesses
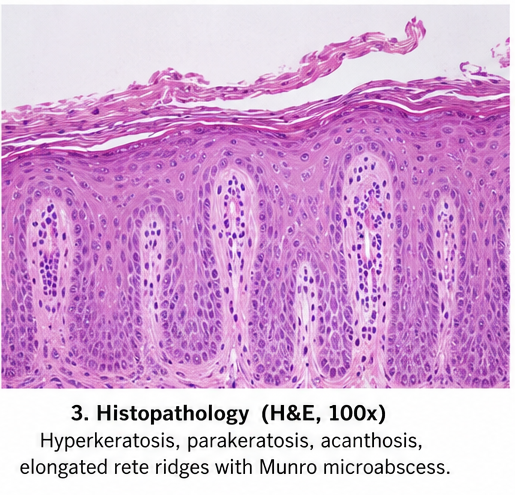
These findings confirmed the diagnosis of psoriasis.
Diagnosis
A definitive diagnosis of scalp psoriasis was established based on characteristic clinical appearance, dermoscopic findings, histopathological confirmation, and exclusion of fungal infection. The presence of sharply defined erythematous plaques covered with thick silvery scales, along with a positive family history and nail pitting, further supported the diagnosis. Histological findings including parakeratosis, acanthosis, and Munro microabscesses were highly consistent with psoriasis vulgaris involving the scalp.
Management and Outcome
Management Strategy
The treatment goals included:
- Reduction of inflammation
- Control of scaling and itching
- Prevention of flare-ups
- Improvement in quality of life
Medical Management
Topical Therapy
The patient was prescribed:
- Topical corticosteroid lotion (clobetasol propionate)
- Vitamin D analogue (calcipotriol)
- Salicylic acid-based keratolytic shampoo
- Coal tar shampoo twice weekly
Supportive Measures
- Avoidance of excessive scratching
- Stress reduction techniques
- Regular scalp moisturization
- Gentle hair care practices
Patient Counseling
The patient was educated regarding:
- Chronic relapsing nature of psoriasis
- Importance of treatment adherence
- Trigger avoidance
- Need for long-term follow-up
Follow-Up
At 4 Weeks
- Significant reduction in itching
- Decrease in scaling
- Improved sleep quality
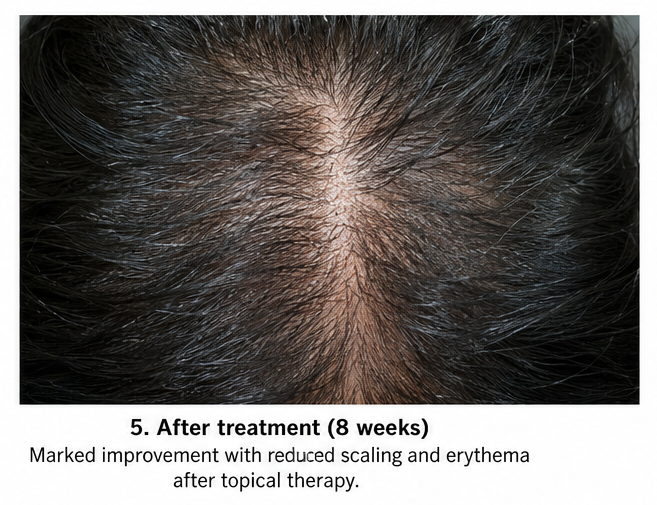
At 8 Weeks
- Marked reduction in erythema
- Plaque thickness reduced considerably
- Hair shedding improved
At 3 Months
- Near-complete resolution of active lesions
- Minimal residual scaling
- Improved psychological confidence and social interaction
No adverse effects related to therapy were noted during follow-up.
Discussion
Pathophysiology
Psoriasis is a T-cell-mediated inflammatory disease characterized by excessive keratinocyte proliferation and altered epidermal differentiation. The disease involves activation of dendritic cells and release of pro-inflammatory cytokines including TNF-α, IL-17, and IL-23, leading to chronic inflammation and epidermal hyperplasia.
In scalp psoriasis, inflammatory activity leads to rapid turnover of epidermal cells, resulting in accumulation of thick scales and erythematous plaques.
Etiology and Risk Factors
Important risk factors include:
- Genetic predisposition
- Family history of psoriasis
- Emotional stress
- Smoking
- Alcohol consumption
- Obesity
- Certain medications
- Infections and trauma
Environmental triggers frequently precipitate disease flare-ups.
Epidemiology
-
Psoriasis affects approximately 2–3% of the global population
- Scalp involvement occurs in nearly 80% of psoriasis patients
- Both genders are equally affected
- Peak onset occurs between 20–50 years of age
- Family history is commonly present
Clinical Manifestations
Common symptoms include:
- Scalp itching
- Thick white scales
- Erythematous plaques
- Burning sensation
- Temporary hair shedding
- Cosmetic and psychological distress
In severe cases, lesions may extend beyond the hairline onto the forehead, neck, and ears.
Diagnostic Considerations
Diagnosis is primarily clinical and supported by:
- Detailed dermatologic examination
- Dermoscopy
- Histopathological evaluation
- Exclusion of fungal infection
Characteristic findings include:
- Well-demarcated plaques
- Silvery scales
- Auspitz sign
- Nail pitting
Treatment Considerations
Topical Therapy
First-line management includes:
- Corticosteroids
- Vitamin D analogues
- Keratolytics
- Coal tar preparations
Phototherapy
Useful in resistant cases:
- Narrowband UVB therapy
- Excimer laser therapy
Systemic Therapy
Indicated in severe or refractory disease:
- Methotrexate
- Cyclosporine
- Acitretin
Biologic Therapy
Advanced therapies target inflammatory cytokines:
- TNF-α inhibitors
- IL-17 inhibitors
- IL-23 inhibitors
These agents have significantly improved disease control in moderate-to-severe psoriasis.
Emerging Therapies
Recent advances include:
- Janus kinase (JAK) inhibitors
- Targeted biologic agents
- Personalized immunotherapy approaches
- Novel topical foam formulations
Research continues to focus on improving long-term efficacy and minimizing adverse effects.
Complications
Potential complications include:
- Secondary bacterial infection
- Sleep disturbance
- Anxiety and depression
- Social embarrassment
- Psoriatic arthritis
- Reduced quality of life
Prognosis
Scalp psoriasis is a chronic relapsing condition with variable severity. Early diagnosis, adherence to therapy, trigger avoidance, and regular follow-up significantly improve long-term outcomes.
Although complete cure remains unavailable, most patients achieve substantial symptom control with appropriate treatment.
Conclusion
Scalp psoriasis is a common chronic inflammatory dermatological condition associated with significant physical discomfort and psychosocial burden. This case emphasizes the importance of early recognition, accurate diagnosis, patient counseling, and individualized treatment planning in achieving effective disease control.
Topical therapy remains the cornerstone of management in mild-to-moderate disease, while systemic and biologic therapies provide effective options for severe or resistant cases. Long-term monitoring and lifestyle modification play critical roles in minimizing relapses and improving patient quality of life.
Advances in immunology and targeted therapies continue to expand therapeutic possibilities for psoriasis management in the future.
References
- Griffiths CEM, Armstrong AW, Gudjonsson JE, Barker JNWN. Psoriasis. https://pubmed.ncbi.nlm.nih.gov/28212781/
- Boehncke WH, Schön MP. Psoriasis. https://pubmed.ncbi.nlm.nih.gov/26450105/
- Rendon A, Schäkel K. Psoriasis Pathogenesis and Treatment. https://pubmed.ncbi.nlm.nih.gov/29484063/
- StatPearls. Scalp Psoriasis. https://www.ncbi.nlm.nih.gov/books/NBK537061/
- Elmets CA, et al. Joint AAD-NPF Guidelines of Care for Psoriasis. https://pubmed.ncbi.nlm.nih.gov/30885733/
- Menter A, et al. Guidelines of care for the management of psoriasis. https://pubmed.ncbi.nlm.nih.gov/18423260/
- Lowes MA, Suárez-Fariñas M, Krueger JG. Immunology of psoriasis. https://pubmed.ncbi.nlm.nih.gov/20967168/
Read more such content on @ Hidoc Dr | Medical Learning App for Doctors
Recommended News For You
Recommended Articles For You
Featured News
Featured Articles
Featured Events
Featured KOL Videos
1.
On all CAR-T products, the FDA is calling for a new boxed warning.
2.
A study has developed molecular markers that predict meningioma recurrence.
3.
Brexpiprazole Safe, Effective in Early-Episode Schizophrenia
4.
AI can identify women at risk of breast cancer years in advance: Study
5.
Advances in TNBC; Mixed News in Lung Cancer Report; Pancreatic Cancer Overdiagnosis?
1.
A Visual Journey Through Penile Cancer: Examining the Impact of Photos
2.
Unleashing the Inner Predator: Reprogramming Macrophages to Conquer Cancer Immunotherapy
3.
Unlocking the Immune Arsenal: A Revolution in Cancer Treatment
4.
The Growing Crisis of Aplastic Anemia: A Call for Action
5.
Interpreting Iron Studies: What Your Blood Results Really Mean
1.
International Lung Cancer Congress®
2.
Genito-Urinary Oncology Summit 2026
3.
Future NRG Oncology Meeting
4.
ISMB 2026 (Intelligent Systems for Molecular Biology)
5.
Annual International Congress on the Future of Breast Cancer East
1.
First Line Combination Therapy- The Overall Survival Data in NSCLC Patients
2.
The Era of Targeted Therapies for ALK+ NSCLC: A Paradigm Shift
3.
INO-VATE: The Long-Term Overall Survival Analysis in Iontuzumab-Treated Patients
4.
Untangling The Best Treatment Approaches For ALK Positive Lung Cancer - Part VIII
5.
Pazopanib Takes Center Stage in Managing Renal Cell Carcinoma - Part III
© Copyright 2026 Hidoc Dr. Inc.
Terms & Conditions - LLP | Inc. | Privacy Policy - LLP | Inc. | Account Deactivation

