Pelvic inflammatory acute disease in a young woman with fever and lower abdominal pain PID
OthersPage Navigation
Abstract
Pelvic inflammatory disease (PID) is a common and potentially serious infection of the upper female genital tract, most often resulting from ascending sexually transmitted pathogens. It predominantly affects young, sexually active women and may lead to long-term sequelae such as infertility, ectopic pregnancy, and chronic pelvic pain if not promptly treated. We report the case of a 24-year-old woman who presented with lower abdominal pain, fever, and purulent cervical discharge. Clinical examination revealed marked cervical motion tenderness, raising strong suspicion for pelvic inflammatory disease. Based on characteristic clinical findings, empirical broad-spectrum antibiotic therapy was initiated, leading to rapid clinical improvement. This case emphasizes the importance of early clinical recognition and timely management of PID in primary care and emergency settings to prevent adverse reproductive outcomes.
Introduction
Pelvic inflammatory disease represents a spectrum of inflammatory disorders involving the uterus, fallopian tubes, ovaries, and adjacent pelvic structures, most commonly caused by ascending infection from the lower genital tract [1]. The condition is frequently associated with sexually transmitted infections, particularly Chlamydia trachomatis and Neisseria gonorrhoeae, although polymicrobial infections involving anaerobes and vaginal flora are also common [2].
PID remains a major public health concern worldwide, particularly among young women of reproductive age. Clinical presentation is often variable, ranging from mild pelvic discomfort to severe abdominal pain with systemic features such as fever, chills, and malaise [3]. Some patients may present with subtle or atypical symptoms, which can complicate timely diagnosis and contribute to underrecognition in clinical practice. Because delayed diagnosis and treatment significantly increase the risk of infertility, ectopic pregnancy, and chronic pelvic pain, a high index of clinical suspicion and early empirical treatment are essential [4].
Early identification in primary care and emergency settings allows prompt initiation of appropriate antimicrobial therapy, reduces the risk of ascending infection, and limits long-term reproductive sequelae. This report describes a classic presentation of PID in a 24-year-old woman and discusses key diagnostic and management considerations relevant to routine clinical practice.
Case Report
Patient History
A 24-year-old woman presented to the outpatient clinic with a 4-day history of progressively worsening lower abdominal pain and fever.
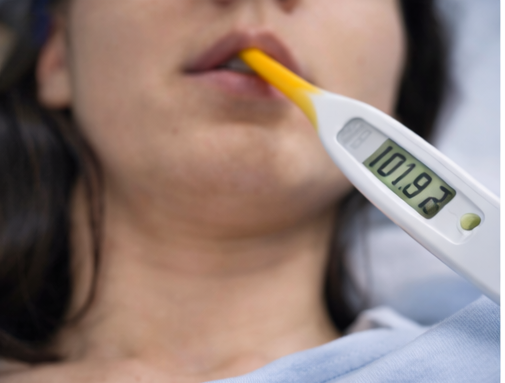
The pain was described as dull, bilateral, and constant, with intermittent exacerbations. She also reported abnormal vaginal discharge that had become thick and foul-smelling over the preceding two days. Associated symptoms included malaise and nausea, but there was no vomiting.
She denied dysuria, flank pain, or gastrointestinal symptoms such as diarrhea. Her menstrual cycles were regular, and her last menstrual period had occurred two weeks prior to presentation. There was no history of recent gynecological procedures, intrauterine device insertion, or previous episodes of similar pain. She reported being sexually active with one partner and inconsistent condom use. There was no known history of sexually transmitted infections.
Clinical Findings
On examination, the patient appeared ill and febrile but was hemodynamically stable.
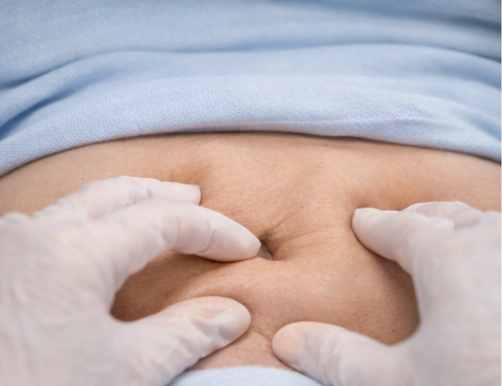
Abdominal examination revealed suprapubic and bilateral lower abdominal tenderness without guarding or rigidity. Bowel sounds were normal.
Pelvic examination demonstrated copious purulent cervical discharge.
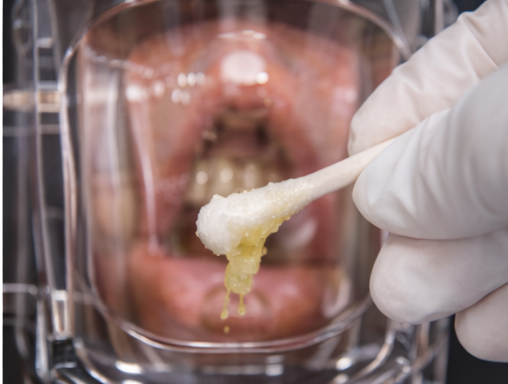
Bimanual examination elicited significant cervical motion tenderness, along with uterine and bilateral adnexal tenderness. No adnexal masses were palpated. These findings were strongly suggestive of pelvic inflammatory disease [1,3].
Investigations
Laboratory investigations showed leukocytosis with neutrophil predominance and elevated inflammatory markers, consistent with an acute infectious process. A urine pregnancy test was negative, excluding ectopic pregnancy. Vaginal and endocervical swabs were obtained for nucleic acid amplification testing for Chlamydia trachomatis and Neisseria gonorrhoeae.
Urinalysis was unremarkable, reducing the likelihood of urinary tract infection. Transvaginal pelvic ultrasonography revealed mild bilateral tubal thickening without evidence of tubo-ovarian abscess or free pelvic fluid. Based on the clinical presentation and supportive findings, a diagnosis of acute pelvic inflammatory disease was established, and treatment was initiated without awaiting microbiological results, in line with current clinical guidelines [2,4].
Management and Outcome
The patient was started on empirical broad-spectrum antibiotic therapy covering likely pathogens, including N. gonorrhoeae, C. trachomatis, anaerobes, and facultative bacteria, as per recommended treatment protocols.
She was advised strict adherence to the antibiotic regimen and counseled on abstaining from sexual activity until completion of treatment and resolution of symptoms. Partner notification and evaluation were also discussed.
Supportive management included antipyretics and analgesics for pain and fever control. Within 72 hours of initiating therapy, the patient reported significant improvement in abdominal pain and resolution of fever. At follow-up after one week, she was clinically stable, asymptomatic, and tolerating oral intake well. No complications were noted, and further counseling regarding safe sexual practices and follow-up screening was provided.
Discussion
Pelvic inflammatory disease results from the ascension of microorganisms from the cervix and vagina to the upper genital tract, leading to inflammation of the endometrium, fallopian tubes, and adjacent structures [2]. Young age, sexual activity, inconsistent barrier contraception, and prior sexually transmitted infections are well-recognized risk factors [3].
The diagnosis of PID is primarily clinical, as no single laboratory or imaging test is sufficiently sensitive or specific to definitively confirm the condition [4]. The presence of lower abdominal pain in a sexually active woman, combined with cervical motion tenderness, uterine tenderness, or adnexal tenderness, constitutes the minimum clinical criteria for diagnosis and warrants prompt empirical treatment [1]. In this case, the combination of fever, purulent cervical discharge, and marked cervical motion tenderness strongly supported the diagnosis.
The differential diagnosis includes ectopic pregnancy, acute appendicitis, ovarian torsion, urinary tract infection, and gastrointestinal conditions such as inflammatory bowel disease [5]. Exclusion of pregnancy and careful clinical evaluation are therefore essential before confirming PID. Early initiation of antibiotic therapy is critical, as treatment delays are directly associated with increased rates of infertility and chronic pelvic pain.
Primary care physicians and gynecologists play a pivotal role in early recognition, treatment initiation, patient education, and partner management. Comprehensive care also includes counseling on sexually transmitted infection prevention and ensuring appropriate follow-up to assess clinical response and prevent recurrence.
Conclusion
Pelvic inflammatory disease is a common but potentially devastating condition affecting young women of reproductive age. This case highlights a classic presentation of PID in a 24-year-old woman with lower abdominal pain, fever, purulent cervical discharge, and cervical motion tenderness. Prompt clinical recognition and early initiation of empirical broad-spectrum antibiotic therapy resulted in rapid symptom resolution and favorable short-term outcomes.
The case underscores the importance of maintaining a high index of suspicion for PID in sexually active women presenting with pelvic pain and systemic symptoms. Early diagnosis, appropriate treatment, partner management, and patient education are essential to reduce morbidity, prevent long-term reproductive complications, and improve overall patient outcomes.
References
- Workowski KA, Bolan GA. Sexually transmitted diseases treatment guidelines. MMWR Recomm Rep. 2015;64(RR-03):1–137.
- Brunham RC, Gottlieb SL, Paavonen J. Pelvic inflammatory disease. N Engl J Med. 2015;372(21):2039–2048.
- Haggerty CL, Ness RB. Diagnosis and treatment of pelvic inflammatory disease. Women’s Health. 2008;4(4):383–397.
- Ross J, Guaschino S, Cusini M, Jensen J. 2017 European guideline for the management of pelvic inflammatory disease. Int J STD AIDS. 2018;29(2):108–114.
- Sweet RL. Pelvic inflammatory disease: current concepts of diagnosis and management. Curr Infect Dis Rep. 2012;14(2):194–203.
Read more such content on @ Hidoc Dr | Medical Learning App for Doctors
Recommended News For You
Recommended Articles For You
Featured News
Featured Articles
Featured Events
Featured KOL Videos
1.
Breast Cancer Patients Living Longer Post-Medicaid Expansion
2.
Error on the MGUS-Autoimmune Disease Association.
3.
Patients with chronic myeloid leukemia who take nilotinib are at higher risk for diabetes and hyperlipidemia.
4.
The majority of cancer medications that receive expedited approval end up failing confirmatory trials.
5.
Unified Neuro/Psych Residency Program: New Proposal.
1.
Optimizing Melanoma Treatment: Strategies in Diagnosis, Clinical Research, and Physician Training
2.
Hemoglobin C: Understanding its Role in Sickle Cell Disease
3.
Beyond the Human Eye: How AI Is Redefining Brain Cancer Diagnosis Through Advanced Imaging
4.
Understanding Abemaciclib: A Breakthrough Treatment for Breast Cancer
5.
The Growing Challenge of Haematological Malignancies in Older Adults
1.
International Lung Cancer Congress®
2.
Genito-Urinary Oncology Summit 2026
3.
Future NRG Oncology Meeting
4.
ISMB 2026 (Intelligent Systems for Molecular Biology)
5.
Annual International Congress on the Future of Breast Cancer East
1.
Revolutionizing Treatment of ALK Rearranged NSCLC with Lorlatinib - Part II
2.
Exploring Potentials of Lorlatinib: The Third Generation ALK-TKI Through CROWN Trial
3.
Molecular Contrast: EGFR Axon 19 vs. Exon 21 Mutations - Part VII
4.
A Conclusive Discussion on CROWN Trial and the Dawn of a New Era in Frontline Management of ALK+ NSCLC
5.
Efficient Management of First line ALK-rearranged NSCLC - Part VI
© Copyright 2026 Hidoc Dr. Inc.
Terms & Conditions - LLP | Inc. | Privacy Policy - LLP | Inc. | Account Deactivation

