Pressure Ulcers (Bed Sores): Clinical Presentation, Diagnostic Evaluation, Management, and Outcomes – A Case Report
OthersPage Navigation
Abstract
Pressure ulcers, also known as bed sores or pressure injuries, are localized damage to the skin and underlying soft tissue resulting from prolonged pressure, shear forces, or friction, most commonly occurring over bony prominences. They are frequently encountered in hospitalized, elderly, and critically ill patients with restricted mobility and are associated with increased morbidity, prolonged hospitalization, and healthcare costs. Clinical presentation varies from non-blanchable erythema to deep tissue necrosis involving muscle and bone. Early diagnosis, accurate staging, and timely multidisciplinary management are crucial to prevent progression and complications such as infection, osteomyelitis, and sepsis. Diagnosis is primarily clinical, supported by laboratory investigations and imaging when deep tissue involvement is suspected. Management strategies include pressure offloading, wound care, nutritional optimization, infection control, and surgical intervention in advanced cases. This case report describes a hospitalized adult patient with a pressure ulcer, emphasizing clinical features, diagnostic evaluation, management approach, and short-term outcomes.
Introduction
Pressure ulcers are a common yet largely preventable complication in hospitalized and long-term care patients, particularly among those with impaired mobility, neurological deficits, advanced age, or chronic illness. They develop when sustained external pressure exceeds capillary perfusion pressure, leading to tissue ischemia, hypoxia, and eventual cell death. Shear forces and friction further exacerbate tissue injury by distorting blood vessels and weakening skin integrity.
Common anatomical sites include the sacrum, heels, hips, ischial tuberosities, and occiput. The severity of pressure ulcers is classified by staging systems such as those proposed by the National Pressure Injury Advisory Panel (NPIAP), ranging from Stage I (intact skin with non-blanchable erythema) to Stage IV (full-thickness skin and tissue loss with exposed bone or muscle). Early-stage ulcers may be subtle and easily overlooked, while advanced lesions can result in serious complications and functional decline.
This case report highlights the evaluation and conservative management of a pressure ulcer in a hospitalized adult patient, underscoring the importance of early recognition and preventive strategies.
Case Report
Patient History
A 72-year-old male patient was admitted to the medical ward following an acute ischemic stroke resulting in right-sided hemiparesis and significantly reduced mobility. The patient had been bedridden for approximately three weeks. His medical history was notable for type 2 diabetes mellitus, hypertension, and chronic kidney disease (stage 3).
During routine nursing assessment, a wound was noted over the sacral region. The patient complained of localized discomfort but denied severe pain, fever, or purulent discharge. There was no prior history of pressure ulcers.
Clinical Examination
On general examination, the patient was hemodynamically stable but appeared frail, with reduced muscle mass and signs of poor nutritional status. Local examination of the sacral area revealed a well-demarcated ulcer measuring approximately 5 × 4 cm. The lesion demonstrated partial-thickness skin loss with a shallow ulcer base, minimal serous discharge, and surrounding erythema without induration or foul odor.
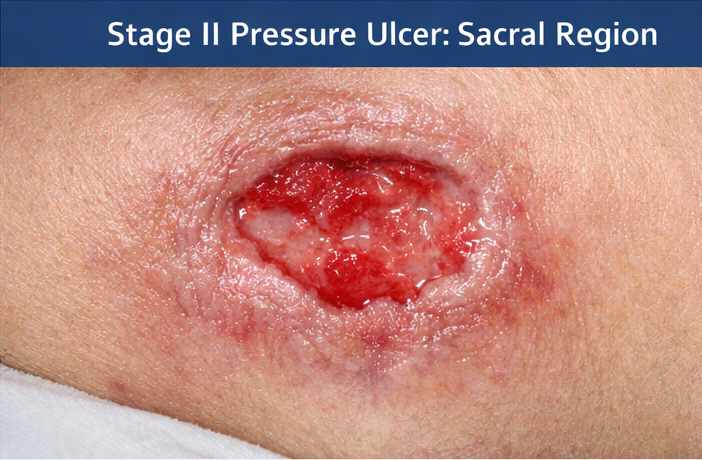
There was no exposure of bone, tendon, or muscle. Based on clinical findings, the lesion was classified as a Stage II pressure ulcer.
Clinical Evaluation
Differential Diagnosis
The differential diagnosis considered included:
• Diabetic skin ulcer
• Ischemic ulcer due to vascular insufficiency
• Infected dermatitis
• Traumatic skin breakdown
The anatomical location, clinical appearance, and history of prolonged immobility strongly favored a diagnosis of pressure ulcer.
Investigations
• Laboratory tests: Mild normocytic anemia; white blood cell count and inflammatory markers within normal limits
• Blood glucose levels: Suboptimal glycemic control
• Serum albumin: Reduced, indicating poor nutritional status
• Wound swab culture: No pathogenic organisms isolated
• Imaging: Not performed, as there were no signs of deep tissue involvement or osteomyelitis
Management and Outcome
Management Strategy
A multidisciplinary management plan was initiated, involving physicians, nurses, and dietitians:
• Pressure offloading: Regular repositioning every two hours and use of a pressure-relieving air mattress
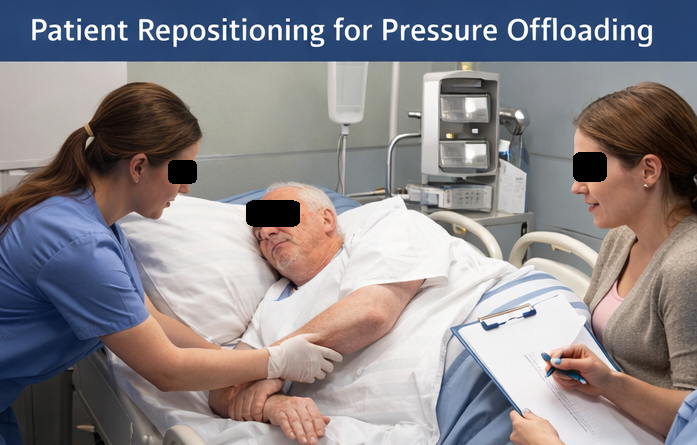

• Local wound care: Gentle cleansing with normal saline and application of moisture-retentive dressings to promote a favorable healing environment
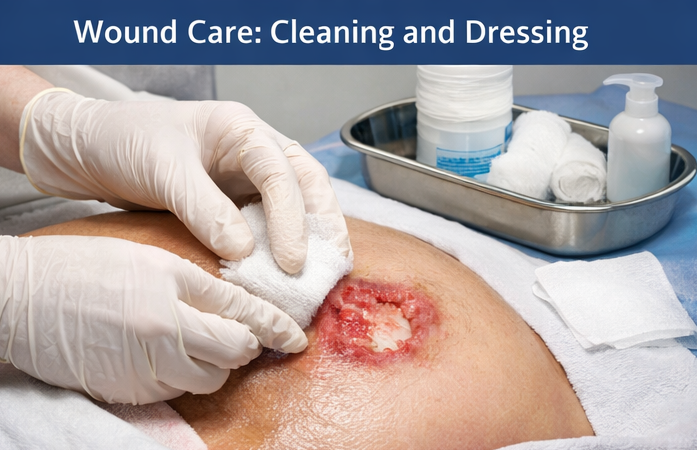
• Nutritional support: High-protein, calorie-dense diet with oral nutritional supplements

• Metabolic control: Optimization of blood glucose levels
• Skin care and hygiene: Maintenance of skin integrity and moisture balance
• Education: Training of caregivers and nursing staff on pressure ulcer prevention
Surgical intervention was not indicated due to the superficial nature of the ulcer.
Follow-Up and Outcome
At two-week follow-up, the ulcer showed healthy granulation tissue and reduction in size, with resolution of surrounding erythema. At six weeks, significant epithelialization was noted, and the wound had nearly healed completely. The patient remained free of secondary infection or systemic complications.
Discussion
Pressure ulcers remain a significant clinical challenge, particularly in hospitalized and immobilized patients. Advanced age, neurological impairment, diabetes, malnutrition, and prolonged bed rest are well-established risk factors. The pathophysiology involves sustained ischemia and reperfusion injury, leading to tissue necrosis.
Clinical assessment and staging guide management decisions. Laboratory investigations and imaging are reserved for suspected complications such as infection or osteomyelitis. Conservative management is effective for early-stage pressure ulcers, focusing on pressure redistribution, wound care, and nutritional optimization.
This case demonstrates that early identification and prompt conservative management can result in favorable outcomes and prevent progression to advanced stages requiring surgical intervention.
Conclusion
Pressure ulcers are common, preventable complications in hospitalized patients with limited mobility. Early recognition, accurate staging, and a multidisciplinary, patient-centered approach are essential for effective management. Conservative treatment of early-stage pressure ulcers can lead to successful healing while minimizing morbidity, healthcare costs, and patient discomfort. Preventive strategies, including regular repositioning, skin assessment, and nutritional support, remain the cornerstone of pressure ulcer care.
References
- National Pressure Injury Advisory Panel. (2019). Prevention and treatment of pressure ulcers/injuries: Clinical practice guideline. https://npiap.com/page/Guidelines
- European Pressure Ulcer Advisory Panel, National Pressure Injury Advisory Panel, & Pan Pacific Pressure Injury Alliance. (2014). Prevention and treatment of pressure ulcers: Clinical practice guideline. https://www.epuap.org/pu-guidelines/
- Thomas, D. R. (2006). Prevention and treatment of pressure ulcers: What works? What doesn’t? JAMA, 296(8), 974–984 https://jamanetwork.com/journals/jama/fullarticle/203324
- Coleman, S., Nixon, J., Keen, J., Wilson, L., McGinnis, E., Dealey, C., … Stubbs, N. (2013). Patient risk factors for pressure ulcer development: Systematic review. International Journal of Nursing Studies, 50(7), 974–1003 https://www.sciencedirect.com/science/article/pii/S0020748912003673
- Jaul, E., & Menzel, J. (2014). Pressure ulcers in the elderly: Clinical and epidemiological aspects. Clinical Interventions in Aging, 9, 177–186 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3906571/
Read more such content on @ Hidoc Dr | Medical Learning App for Doctors
Recommended News For You
Recommended Articles For You
Featured News
Featured Articles
Featured Events
Featured KOL Videos
1.
Researchers find distinct cell receptors with the potential for new treatments.
2.
Breast cancer patients' arms swell less after an effective lymph node transfer.
3.
Telehealth in the pandemic era resulted in fewer therapy interruptions.
4.
Too Many Chest CTs for Incidental Lung Nodules?
5.
Global warming could be driving up women's cancer risk, find researchers
1.
The New Frontier of Cancer Survivorship: Navigating the Long-Term Effects of Immunotherapy and Targeted Therapies
2.
Deterministic Reprogramming of Neutrophils within Tumors: A New Frontier in Cancer Research
3.
Neuroendocrine Tumors: Case Study on Diagnosis, Treatment Strategies & Patient Management
4.
Ticagrelor Monotherapy vs. Ticagrelor + Aspirin in ACS Post-PCI: ULTIMATE-DAPT Trial
5.
Transfusing the Future: Exploring the Possibilities of Blood Transfusions
1.
International Lung Cancer Congress®
2.
Genito-Urinary Oncology Summit 2026
3.
Future NRG Oncology Meeting
4.
ISMB 2026 (Intelligent Systems for Molecular Biology)
5.
Annual International Congress on the Future of Breast Cancer East
1.
Current Scenario of Blood Cancer- A Conclusion on Genomic Testing & Advancement in Diagnosis and Treatment
2.
Navigating the Brain Barrier: The CNS Challenge in ALK+ NSCLC
3.
Thromboprophylaxis In Medical Settings
4.
Treatment Paradigm for Patients with R/R Adult B-cell ALL- Expert Discussions
5.
Current Scenario of Blood Cancer- Genomic Testing & Advancement in Diagnosis and Treatment
© Copyright 2026 Hidoc Dr. Inc.
Terms & Conditions - LLP | Inc. | Privacy Policy - LLP | Inc. | Account Deactivation

