Rabies Encephalitis in a Child Following Dog Bite: A Clinicopathological Case Report
OthersPage Navigation
Abstract
Rabies is an acute, progressive, and almost universally fatal viral encephalitis caused by the rabies virus, a member of the Lyssavirus genus. Despite being preventable through timely post-exposure prophylaxis, rabies remains a major public health problem in many low- and middle-income countries, particularly affecting children. The disease is characterized by a prolonged incubation period followed by rapid neurological deterioration once clinical symptoms appear.
We report a fatal case of rabies in a 10-year-old boy following a dog bite, with diagnosis confirmed by the demonstration of Negri bodies in brain tissue. This case underscores the importance of early wound management, timely administration of post-exposure prophylaxis, challenges in clinical diagnosis, and the critical role of preventive strategies, including animal vaccination and public awareness.
Introduction
Rabies is a zoonotic viral disease transmitted primarily through the bite of infected mammals, most commonly dogs. The rabies virus is a neurotropic, single-stranded RNA virus that causes progressive encephalomyelitis once it reaches the central nervous system. Globally, rabies accounts for an estimated 59,000 deaths annually, with children under 15 years constituting a substantial proportion of cases [1].
Although rabies is preventable through prompt post-exposure prophylaxis (PEP), delayed presentation, lack of awareness, and inadequate access to healthcare continue to contribute to rabies-related mortality. Once clinical symptoms manifest, the disease is almost invariably fatal. Classic pathological findings include intracytoplasmic eosinophilic inclusions known as Negri bodies, typically found in neurons of the hippocampus and cerebellum [2].
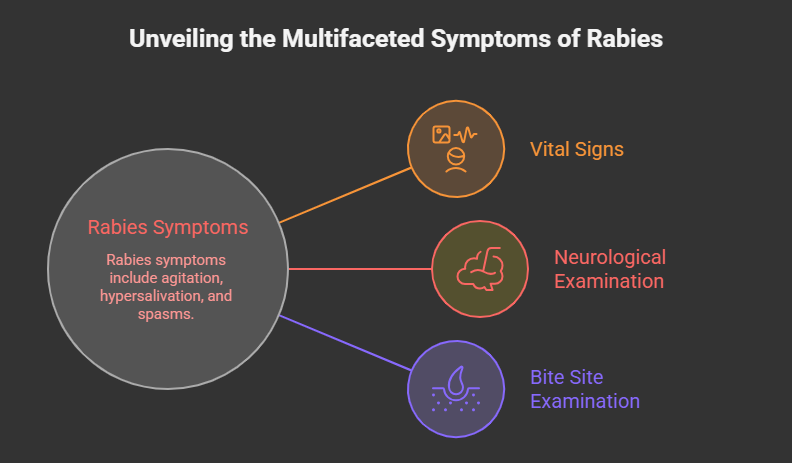
This case report describes the clinical presentation, diagnostic confirmation, and outcome of rabies in a pediatric patient following a dog bite, highlighting missed opportunities for prevention and the need for strengthened public health measures.
Case Report
Patient History
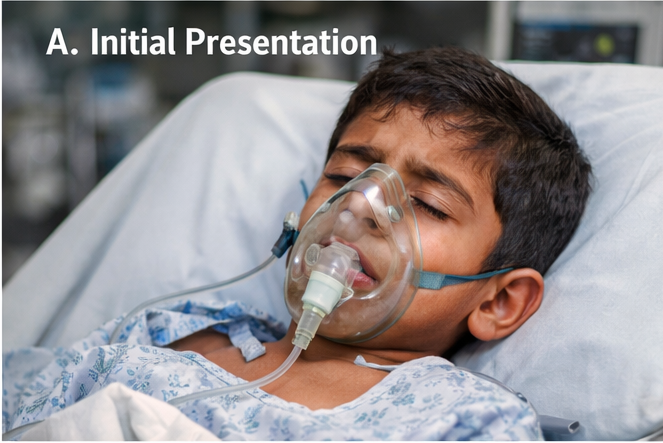
A 10-year-old boy was brought to the emergency department with complaints of fever, agitation, difficulty swallowing, and episodic involuntary movements for two days. The child had been previously healthy, with no known chronic medical illnesses.
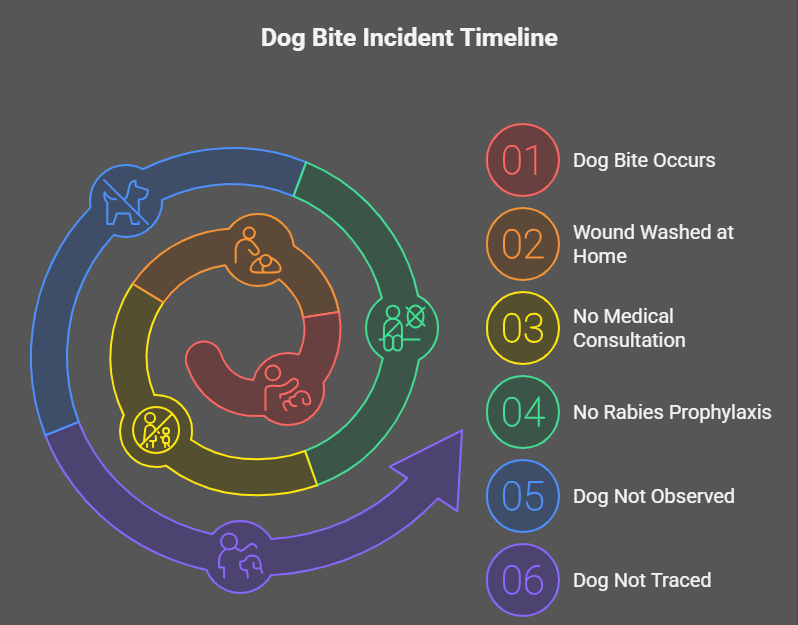
A detailed history revealed that the child had sustained a bite on his right lower leg by a stray dog approximately six weeks prior to presentation. The wound was reportedly superficial and was washed at home with water. No medical consultation was sought at that time, and no rabies post-exposure prophylaxis, including rabies vaccination or rabies immunoglobulin, was administered. The dog was not observed after the incident and could not be traced.
Clinical Examination
On admission, the child appeared acutely ill, anxious, and restless. Vital signs revealed a temperature of 38.8°C, heart rate of 120 beats per minute, blood pressure of 98/60 mmHg, and respiratory rate of 24 breaths per minute. Oxygen saturation was 96% on room air.
Neurological examination showed marked agitation, hypersalivation, and intermittent muscle spasms. Attempts to give oral fluids provoked painful pharyngeal spasms, consistent with hydrophobia. Aerophobia was also noted when air currents triggered distress and spasms. The Glasgow Coma Scale score was 12/15.
Examination of the bite site revealed a healed scar on the right lower leg with no signs of active infection. Cardiovascular, respiratory, and abdominal examinations were otherwise unremarkable.
Clinical Evaluation
Initial Differential Diagnosis
Based on the clinical presentation and history of animal bite, the following differential diagnoses were considered:
• Rabies encephalitis
• Viral meningoencephalitis
• Acute bacterial encephalitis
• Tetanus
• Autoimmune encephalitis
Given the characteristic features of hydrophobia, aerophobia, hypersalivation, and a history of dog bite, rabies was considered the most likely diagnosis.
Investigations
Laboratory Studies
Routine laboratory investigations revealed mild leukocytosis. Serum electrolytes, renal function tests, and liver function tests were within normal limits. Cerebrospinal fluid analysis showed mild lymphocytic pleocytosis with elevated protein levels, findings consistent with viral encephalitis but not specific for rabies.
Neuroimaging
Magnetic resonance imaging (MRI) of the brain demonstrated diffuse cerebral edema with hyperintense signals in the brainstem and basal ganglia on T2-weighted and FLAIR sequences, suggestive of encephalitis.
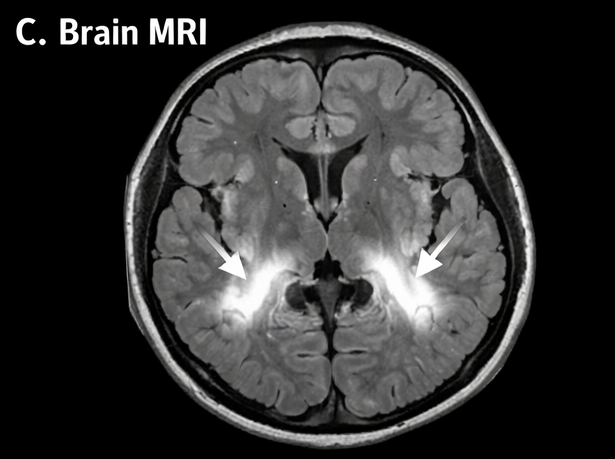
Diagnosis
Despite supportive care, the patient’s neurological status deteriorated rapidly, progressing to coma within 48 hours of admission. The child developed autonomic instability and respiratory failure, necessitating mechanical ventilation.
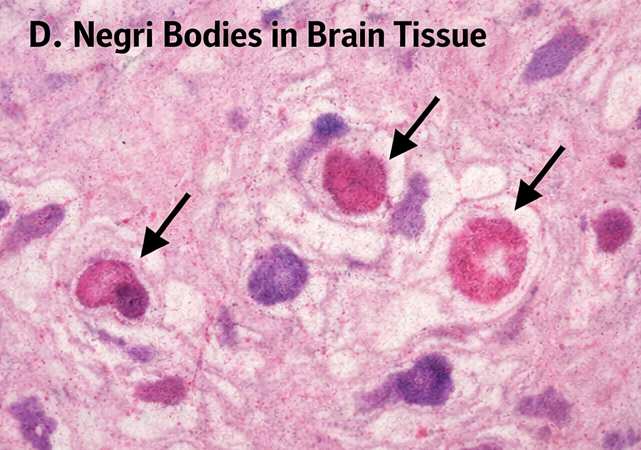
The patient succumbed to the illness on the fifth day of hospitalization. Post-mortem examination of brain tissue was performed. Histopathological analysis revealed the presence of characteristic intracytoplasmic eosinophilic inclusion bodies (Negri bodies) within neurons of the hippocampus and cerebellum, confirming the diagnosis of rabies encephalitis.
The diagnosis was established based on clinical presentation, epidemiological history, and definitive pathological confirmation.
Management and Outcome
Therapeutic Management
Management was primarily supportive, focusing on sedation, control of agitation and seizures, airway protection, and maintenance of hemodynamic stability. The patient was isolated, and barrier nursing precautions were implemented.
No specific antiviral therapy has been proven effective once clinical rabies develops. Rabies post-exposure prophylaxis was not initiated at this stage, as it is ineffective after symptom onset.
Outcome
Despite aggressive supportive management in the intensive care unit, the patient’s condition continued to worsen, culminating in death due to cardiorespiratory failure. The fatal outcome was consistent with the known natural history of symptomatic rabies.
Discussion
Rabies remains one of the deadliest infectious diseases, with near-100% mortality once clinical symptoms appear. Children are particularly vulnerable due to increased exposure to animals and delayed reporting of bites. This case illustrates the classical presentation of rabies, including hydrophobia, aerophobia, and rapid neurological decline.
The long incubation period, typically ranging from weeks to months, offers a critical window for intervention through post-exposure prophylaxis. Immediate wound cleansing, administration of rabies vaccine, and infiltration of rabies immunoglobulin are highly effective in preventing disease if given promptly [3].
Negri bodies, though not always present, remain a hallmark pathological finding and provide definitive evidence of rabies infection. The presence of these inclusions reflects viral replication within neurons and advanced disease progression [4].
This case highlights missed opportunities for prevention and underscores the need for community education regarding dog bite management, improved access to rabies vaccines, and robust animal control programs.
Conclusion
Rabies is a preventable yet fatal disease once clinical manifestations develop. Any dog bite, particularly in children, should be treated as a medical emergency requiring immediate wound care and post-exposure prophylaxis. This case emphasizes the importance of early intervention, public awareness, and coordinated public health strategies to eliminate rabies-related mortality. Strengthening vaccination coverage in both human and animal populations remains essential to achieving rabies elimination goals.
References
- World Health Organization. Rabies fact sheet. WHO; 2023.
- Jackson AC. Rabies: scientific basis of the disease and its management. Lancet. 2013;381(9863):443–452.
- Rupprecht CE, et al. Human rabies prevention—United States, 2008. MMWR Recomm Rep. 2008;57(RR-3):1–28.
- Hemachudha T, et al. Human rabies: neuropathogenesis, diagnosis, and management. Lancet Neurol. 2013;12(5):498–513.
Read more such content on @ Hidoc Dr | Medical Learning App for Doctors
Recommended News For You
Recommended Articles For You
Featured News
Featured Articles
Featured Events
Featured KOL Videos
1.
Data indicate 1 in 3 US adults unaware of connection between HPV and cancers
2.
Early Esophageal Cancer pCR Rates Are Raised by Neoadjuvant PD-1 Blockade.
3.
New imaging probe helps track prostate cancer and possibly treat it before resistance develops
4.
A novel blood test may enable the early identification of common, fatal cancers.
5.
Children living near oil and gas wells face higher risk of rare leukemia, studies show
1.
What You Need to Know About the Early Warning Signs of Colon Cancer
2.
Uncovering the Hidden Picture: Using Ultrasound to Diagnose Breast Cancer
3.
Unlocking the Potential of Red Bone Marrow in the Formation of Blood Cells
4.
Unlocking the Potential of Reticulocytes: The Key to Enhanced Blood Production
5.
Unlocking the Potential of Polatuzumab for Cancer Treatment
1.
International Lung Cancer Congress®
2.
Genito-Urinary Oncology Summit 2026
3.
Future NRG Oncology Meeting
4.
ISMB 2026 (Intelligent Systems for Molecular Biology)
5.
Annual International Congress on the Future of Breast Cancer East
1.
Navigating the Complexities of Ph Negative ALL - Part X
2.
Navigating the Complexities of Ph Negative ALL - Part XII
3.
A Comprehensive Guide to First Line Management of ALK Positive Lung Cancer - Part VII
4.
Role of Nimotuzumab in Management of Nasopharyngeal Cancer
5.
Managing ALK Rearranged Non-Small Cell Lung Cancer with Lorlatinib - Part II
© Copyright 2026 Hidoc Dr. Inc.
Terms & Conditions - LLP | Inc. | Privacy Policy - LLP | Inc. | Account Deactivation

