Dyshidrotic Eczema (Pompholyx): Clinical Features, Diagnostic Challenges, and Management - A Case Report
OthersPage Navigation
Abstract
Dyshidrotic eczema, also known as pompholyx or vesicular palmoplantar eczema, is a chronic, relapsing inflammatory dermatosis characterized by pruritic vesicles on the palms, soles, or both. The condition is often associated with significant morbidity due to pain, itching, functional impairment, and recurrent flares. Although its exact etiology remains unclear, factors such as atopy, contact allergens, stress, hyperhidrosis, and environmental triggers are implicated.
We report a case of dyshidrotic eczema in a middle-aged patient presenting with recurrent vesicular eruptions over the palms, highlighting the clinical presentation, diagnostic considerations, therapeutic approach, and outcome. This case emphasizes the importance of accurate diagnosis, trigger identification, and a multidisciplinary management strategy to improve patient quality of life.
Introduction
Dyshidrotic eczema is a distinct form of eczema predominantly affecting the palms and soles. It accounts for a significant proportion of hand and foot dermatitis cases encountered in dermatology practice. The disease is characterized by sudden onset of deep-seated, clear vesicles often described as having a “tapioca pudding” appearance, accompanied by intense pruritus or burning sensation.
The condition follows a chronic relapsing course and can substantially impair daily activities, occupational performance, and psychosocial well-being. Despite its recognizable clinical appearance, dyshidrotic eczema may be misdiagnosed as fungal infection, contact dermatitis, or palmoplantar psoriasis. This case report aims to describe a typical presentation of dyshidrotic eczema, discuss diagnostic challenges, and outline evidence-based management strategies.
Case Report
Patient History
A 38-year-old woman presented to the dermatology outpatient clinic with a 6-month history of recurrent itchy eruptions on both palms. The lesions appeared episodically, often worsening during periods of emotional stress and hot weather. Each episode lasted approximately 2–3 weeks and partially resolved with over-the-counter topical creams, only to recur.
The patient reported intense pruritus and a burning sensation, leading to scratching and discomfort during routine activities such as writing and household work. There was no history of similar lesions elsewhere on the body. She had a past history of allergic rhinitis but denied asthma or atopic dermatitis in childhood.
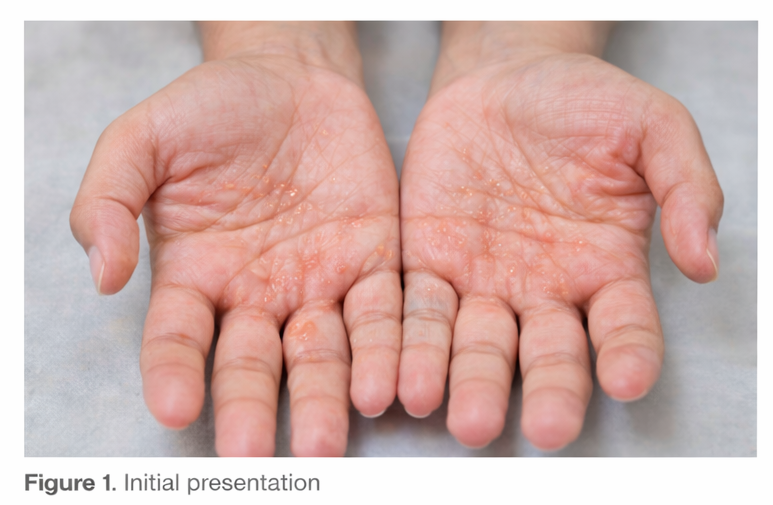
No significant drug history was noted. There was no known contact with chemicals, although the patient frequently used detergents without gloves. Family history was non-contributory.
Clinical Examination
On examination, multiple symmetrical, deep-seated vesicles were observed over the central palms and lateral aspects of the fingers of both hands. The vesicles were small, tense, and translucent, with minimal surrounding erythema. Some areas showed mild scaling and post-inflammatory hyperpigmentation, suggesting resolving lesions.
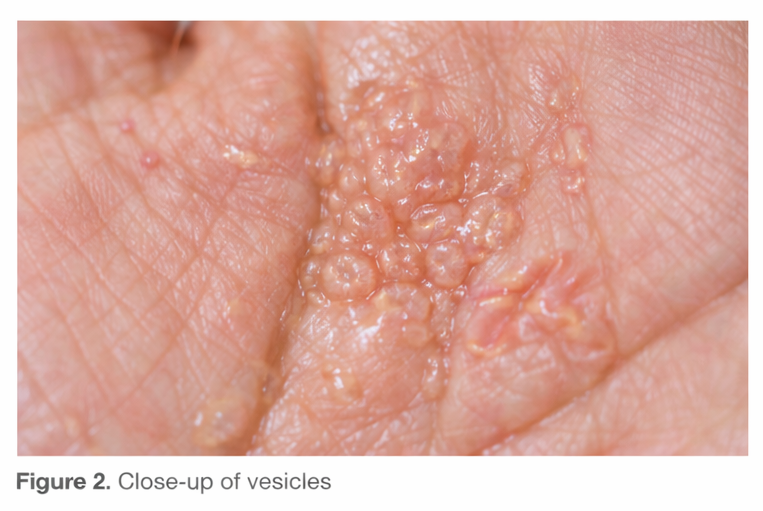
There were no signs of secondary bacterial infection. The soles, nails, scalp, and mucous membranes were normal. Systemic examination was unremarkable.
Clinical Evaluation
Differential Diagnosis
Based on the clinical presentation, the following differential diagnoses were considered:
- Dyshidrotic eczema (pompholyx)
- Allergic contact dermatitis
- Irritant contact dermatitis
- Tinea manuum
- Palmoplantar psoriasis
The symmetrical distribution, recurrent vesicular pattern, absence of well-demarcated plaques, and lack of nail involvement favored a diagnosis of dyshidrotic eczema.
Investigations
Laboratory Studies
Routine hematological and biochemical parameters were within normal limits. Serum IgE levels were mildly elevated, consistent with an atopic tendency.

Mycological Examination
Potassium hydroxide (KOH) preparation from vesicular fluid and skin scrapings was negative for fungal elements, excluding dermatophytosis.
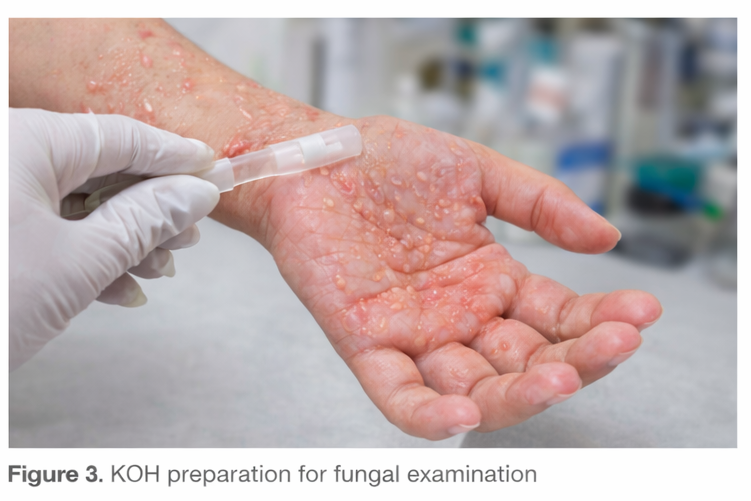
Patch Testing
Patch testing was advised to evaluate possible contact allergens. The patient showed mild sensitivity to nickel sulfate, suggesting a contributory role of contact allergy.
Diagnosis
The diagnosis of dyshidrotic eczema was established based on clinical features, exclusion of fungal infection, and supportive history of atopy and trigger factors such as stress and detergent exposure.
Management and Outcome
Therapeutic Management
The patient was managed with a combination of pharmacological and non-pharmacological measures:
- Topical therapy:
- High-potency topical corticosteroid applied once daily for two weeks
- Emollients applied liberally to restore skin barrier function
- Systemic therapy:
- Oral antihistamines to control pruritus
- Supportive measures:
- Avoidance of irritants and allergens, including detergents and nickel-containing objects
- Use of protective gloves during wet work
- Stress management counseling
The patient was educated about the chronic relapsing nature of the disease and the importance of adherence to therapy and trigger avoidance.
Outcome
Significant clinical improvement was noted within two weeks, with resolution of vesicles and marked reduction in pruritus. At a 3-month follow-up, the patient reported only one mild flare, which responded promptly to topical therapy. Overall functional ability and quality of life improved substantially.
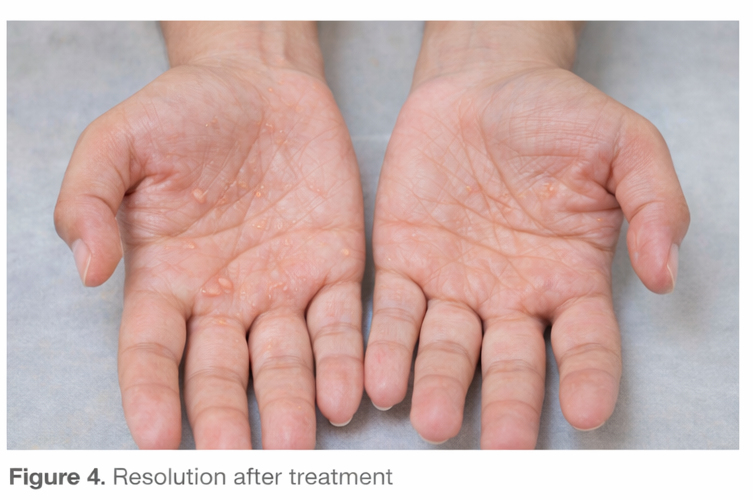
Discussion
Dyshidrotic eczema is a common yet often under-recognized dermatological condition. Although previously thought to be related to sweat gland dysfunction, current evidence suggests a multifactorial etiology involving genetic predisposition, immune dysregulation, contact allergens, and environmental factors.
Atopy is a well-established risk factor, as seen in this patient with allergic rhinitis and elevated IgE levels. Contact allergens such as nickel can exacerbate or trigger episodes, underscoring the role of patch testing in recurrent or refractory cases.
Clinically, dyshidrotic eczema is distinguished by its characteristic vesicles and distribution. However, overlap with other palmoplantar dermatoses necessitates careful evaluation. Exclusion of fungal infection is particularly important, as misdiagnosis may lead to inappropriate treatment.
Management focuses on symptom control, reduction of inflammation, and prevention of recurrences. Topical corticosteroids remain the mainstay of treatment, while emollients play a critical role in maintaining skin barrier integrity. In severe or refractory cases, systemic therapies such as oral corticosteroids, immunosuppressants, or phototherapy may be required.
This case highlights the importance of a holistic approach, incorporating patient education, trigger identification, and long-term management strategies.
Conclusion
Dyshidrotic eczema is a chronic, relapsing condition that can significantly impair quality of life if not appropriately managed. Accurate diagnosis, exclusion of mimicking conditions, and identification of triggering factors are essential for effective treatment. Early intervention, patient education, and adherence to preventive measures can lead to favorable outcomes and reduced disease burden.
When promptly recognized and managed with a combination of topical therapies, trigger avoidance, and lifestyle modifications, many patients experience prolonged remission. A structured, individualized treatment approach not only minimizes flare frequency and severity but also improves long-term skin health and overall patient well-being.
References
- Lofgren SM, Warshaw EM. Dyshidrosis: epidemiology, clinical characteristics, and therapy. Dermatitis. 2006;17(4):165–181.
- Meding B, Swanbeck G. Epidemiology of different types of hand eczema in an industrial city. Acta Derm Venereol. 1989;69(3):227–233.
- Alinaghi F, et al. Atopic dermatitis and risk of hand eczema: a systematic review. J Am Acad Dermatol. 2018;78(2):362–369.
- Thyssen JP, et al. Causes of hand eczema. Contact Dermatitis. 2010;62(2):75–87.
Read more such content on @ Hidoc Dr | Medical Learning App for Doctors
Recommended News For You
Recommended Articles For You
Featured News
Featured Articles
Featured Events
Featured KOL Videos
1.
Babies Are Bleeding to Death as Parents Reject a Vitamin Shot Given at Birth
2.
Detecting pancreatic cancer through changes in body composition and metabolism
3.
In heavily pretreated DLBCL, Triplet Scores a Survival Victory.
4.
The pandemic had little impact on mental health symptoms.
5.
Men over 75 years old may be significantly more likely to commit suicide if they have cancer.
1.
From Muscle Soreness to Improved Endurance: The Benefits of Monitoring Lactic Acid Levels
2.
Unlocking the Mystery of Basilar Artery Stroke: A New Approach to Treatment
3.
Intrapancreatic Fat, Pancreatitis, and Cancer: Role of Cancer-Associated Fibroblasts
4.
Understanding Acute Intermittent Porphyria: Symptoms, Diagnosis and Treatment
5.
Exploring the Unknown: Unveiling the Mysteries of GIST Tumors
1.
International Lung Cancer Congress®
2.
Genito-Urinary Oncology Summit 2026
3.
Future NRG Oncology Meeting
4.
ISMB 2026 (Intelligent Systems for Molecular Biology)
5.
Annual International Congress on the Future of Breast Cancer East
1.
Treatment Sequencing Strategies in ALK + NSCLC Patients with CNS Diseases - Part II
2.
Managing ALK Rearranged Non-Small Cell Lung Cancer with Lorlatinib - Part II
3.
Virtual Case Study on Deep Vein Thrombosis (DVT) - An Initiative by Hidoc Dr.
4.
From Relapse to Remission : Chasing the Invisible and Redefining Long-Term Survival in Adult R/R B-Cell ALL
5.
Pazopanib: A Game-Changer in Managing Advanced Renal Cell Carcinoma - Part IV
© Copyright 2026 Hidoc Dr. Inc.
Terms & Conditions - LLP | Inc. | Privacy Policy - LLP | Inc. | Account Deactivation

